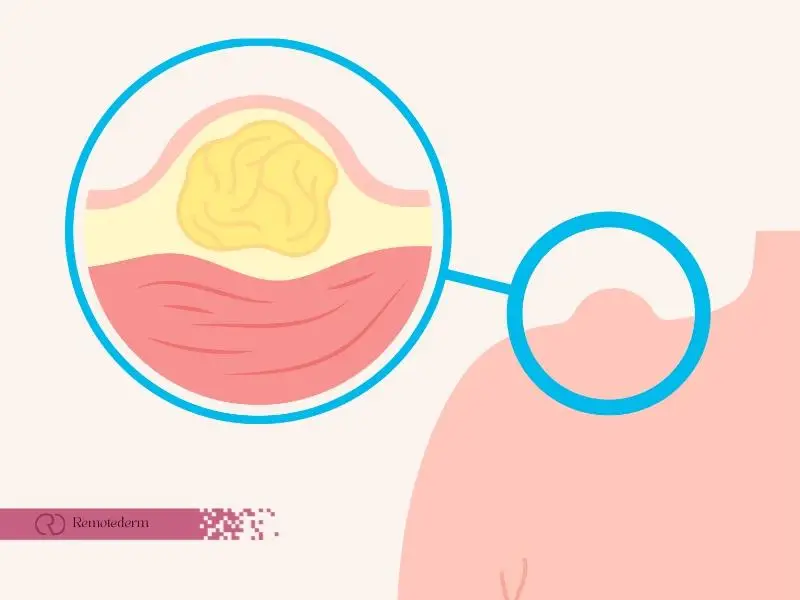
Are you concerned about those mysterious bumps and lumps on your skin? It’s a common dilemma many individuals face, and they might be dealing with epidermal inclusion cysts. In this comprehensive guide, we’ll delve into the intricacies of epidermal inclusion cysts, also known as epidermoid inclusion cysts, their causes, symptoms, and effective treatments. So, let’s embark on this journey to better understand these enigmatic skin issues.
Understanding Epidermal Inclusion Cysts
Epidermal inclusion cysts, often referred to as epidermoid inclusion cysts or simply inclusion cysts, are benign skin growths that can develop in various areas of the body. These cysts typically originate from hair follicles and are often filled with keratin, a protein found in hair and skin. They can appear as small, round lumps beneath the skin’s surface, usually ranging in size from a pea to a marble.
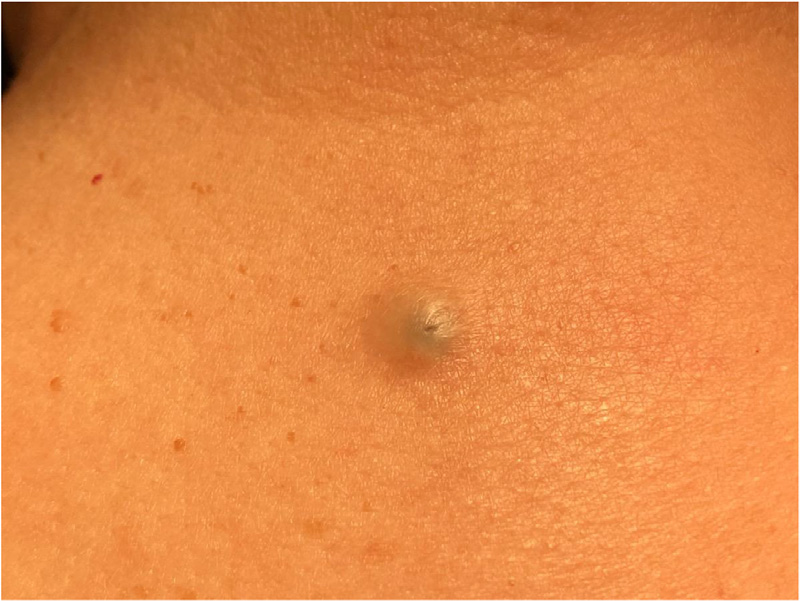
What Causes Epidermal Inclusion Cysts?
The precise etiology of epidermal inclusion cysts is frequently unknown; however, there are several common factors that are known to be associated with their genesis:
- Hair Follicle Blockage: A primary catalyst behind the formation of these cysts stems from the obstruction of hair follicles. This obstruction may result from the accumulation of dirt, sebum (skin oil), or the shedding of dead skin cells.
- Trauma or Injury: In certain instances, physical trauma or injury to the skin can serve as a trigger for the development of an inclusion cyst. This phenomenon is particularly noteworthy in areas of the body prone to recurrent friction or irritation.
- Genetic Predisposition: A hereditary component plays a role in some cases, as certain individuals may have a genetic predisposition to the development of inclusion cysts. If there is a history of such cysts within your family, it can elevate your risk of experiencing them as well.
- Chronic Skin Conditions: Certain enduring skin conditions, most notably acne, can increase your susceptibility to the occurrence of inclusion cysts. The ongoing presence of conditions like acne can create an environment conducive to the development of these cysts.
Identifying the Symptoms
Epidermal inclusion cysts, though typically characterized by their painless nature, can manifest a spectrum of symptoms that are essential to acknowledge and comprehend. These symptoms include:
- Visible Bumps on the Skin: The most conspicuous and readily detectable indicator of an epidermal inclusion cyst is the presence of a discernible bump on the surface of the skin. These bumps are usually of a modest size and are palpable just beneath the skin’s outermost layer. Their tactile presence often serves as the initial sign that something may be amiss.
- Skin Redness and Inflammation: In certain instances, the vicinity surrounding the cyst may undergo a change in appearance and texture, resulting in skin redness and inflammation. This inflammatory response is a reactive element to the presence of the cyst and may be accompanied by mild discomfort or irritation.
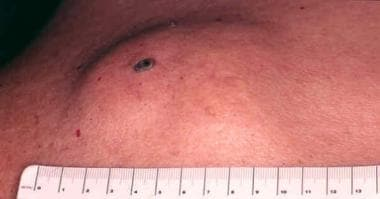
Identifying the Symptoms of epidermal inclusion cyst
epidermal inclusion cyst Symptoms
- Thick, Yellow, and Unpleasant Discharge: Should the epidermal inclusion cyst become infected, it has the potential to generate a thick, yellow, and malodorous discharge. This discharge is a consequential outcome of the infection and can contribute to localized discomfort or heightened awareness of the cyst’s presence.
- Altered Sensations in the Skin: Periodically, the skin overlying the cyst may exhibit anomalous sensations. It might feel warmer to the touch compared to the surrounding skin, and there may be a degree of tenderness or discomfort experienced in the region. These altered sensations can be indicative of the cyst’s influence on the surrounding tissues.
Effective Treatment Options
The management of epidermal inclusion cysts necessitates a nuanced approach, as treatment choices are contingent upon factors such as the cyst’s severity, size, and the degree of discomfort experienced. These treatment modalities can be broadly categorized into two primary approaches:
Non-Invasive Treatment Options
These methods aim to either allow the cyst to naturally regress or address issues like inflammation and infection without resorting to invasive procedures:
- Observation: In cases where the cyst is relatively small, asymptomatic, and poses no significant discomfort or medical concern, a dermatologist may recommend a strategy of vigilant observation. This entails periodic monitoring of the cyst’s status without immediate medical intervention, as some cysts may remain dormant or even regress over time.
- Warm Compress Therapy: A non-invasive technique that can be employed involves the application of a warm compress to the cyst. The application of heat via a warm compress serves to mitigate inflammation and can stimulate the cyst to drain spontaneously. This approach is particularly applicable when the cyst is not accompanied by signs of infection.
- Antibiotic Treatment: In situations where an epidermal inclusion cyst has become infected, your healthcare provider may opt for a course of antibiotic therapy. Antibiotics are administered to combat the infection, with the aim of resolving the infectious process before contemplating more invasive interventions.
Invasive Treatment Approaches:
Invasive treatments are typically recommended when the cyst’s size, symptoms, or infection require more direct intervention. These approaches aim to efficiently address the cyst and its associated issues:
- Incision and Drainage: An invasive procedure called “incision and drainage” involves the creation of a small incision in the cyst, facilitating the release of its contents. Typically carried out by a dermatologist in a sterile clinical setting, this method is primarily employed when the cyst exhibits signs of infection, pain, or substantial inflammation.
- Cyst Removal Surgery: When an epidermal inclusion cyst is sizable, painful, recurrent, or prone to infection, surgical excision becomes the preferred course of action. This surgical removal of the cyst is performed under local anesthesia, ensuring the patient’s comfort and minimal discomfort during the procedure. It is a definitive solution to address the cyst’s presence and minimize the risk of recurrence.
- Laser Therapy: In certain specific cases, healthcare providers may explore the option of laser therapy as a less invasive means of cyst removal. Laser therapy is precise and entails minimal invasiveness, making it an attractive choice for some patients. This method utilizes focused laser energy to eliminate the cyst’s contents and its cystic wall.
Seeking Online Dermatology Assistance
In this digital age, seeking professional guidance has become easier than ever. Thanks to online dermatology services, you can now consult with a certified dermatologist from the comfort of your home. These platforms provide a convenient and efficient way to address your skin concerns.
Final Thoughts
Epidermal inclusion cysts, also referred to as epidermoid inclusion cysts, are a perplexing skin condition. While they may appear as harmless skin protrusions, they conceal a world of complexity. It’s crucial to understand these cysts, including their causes, symptoms, and treatment options, for anyone who may encounter them. These cysts can originate from various factors like hair follicle blockages, physical trauma, genetic predisposition, and chronic skin conditions. Identifying their symptoms, which can range from visible skin irregularities to signs of inflammation and potential infection, empowers individuals to recognize and seek medical attention when necessary.
Treatment options vary, from non-invasive methods like observation and warm compress therapy to more invasive procedures like incision and drainage, cyst removal surgery, or laser therapy, depending on the individual’s situation. Online dermatology services offer a convenient means of obtaining expert guidance and tailored treatment recommendations. In navigating the realm of epidermal inclusion cysts, knowledge, awareness, and professional support are essential for promoting skin health and overall well-being.
FAQs
- Are epidermal inclusion cysts common?
Yes, these cysts are relatively common and can affect individuals of all ages.
- How are epidermal inclusion cysts diagnosed?
A dermatologist typically diagnoses these cysts through a physical examination and, if necessary, imaging tests.
- Can an epidermal inclusion cyst be popped or squeezed?
It’s not advisable to attempt popping or squeezing these cysts, as it can lead to infection, scarring, and further complications.
- What should I do if I suspect I have an epidermal inclusion cyst?
If you notice a cyst on your skin or experience symptoms, it’s advisable to consult a healthcare professional for proper evaluation and guidance.