Melasma is one of the most common skin conditions. It causes brown or gray patches to appear on the face, particularly on the cheeks, forehead, nose, chin, and above the upper lip. The condition is more prevalent in women than men, and it is often associated with pregnancy, hormonal changes, or sun exposure. In this article, we will discuss in detail the causes, treatment options, and how to prevent melasma.
What is Melasma?
Melasma is one of skin diseases that causes dark patches on the face, particularly on the cheeks, forehead, nose, and upper lip. The patches are usually brown or gray in color and can vary in size and shape. Melasma is most common in women, especially those who are pregnant or taking birth control pills. However, men can also develop melasma, although it is less common.

What Causes Melasma?
While the exact cause of melasma is not fully understood, there are several factors that are believed to contribute to the development of this condition. Some of the factors that are known to cause melasma include:
- Hormonal changes: Melasma is often associated with hormonal changes, particularly in women. This may include changes that occur during pregnancy, menopause, or when using hormonal birth control.
- Sun exposure: Exposure to UV radiation from the sun is known to trigger the development of melasma, and the condition is more common in individuals with darker skin tones.
- Genetic predisposition: There is evidence to suggest that genetics may play a role in the development of melasma. Individuals with a family history of melasma are more likely to develop the condition themselves.
- Skin irritation: Certain skincare products or cosmetic procedures can irritate the skin and trigger the development of melasma.
- Medications: Certain medications, such as anticonvulsants and hormone replacement therapy, have been associated with an increased risk of developing melasma.
Several studies have examined the underlying causes of melasma. One study published in the Journal of the European Academy of Dermatology and Venereology found that melasma is associated with increased activity of melanocytes, the cells responsible for producing melanin. Another study published in the Journal of Investigative Dermatology found that the overproduction of a protein called endothelin-1 may play a role in the development of melasma.
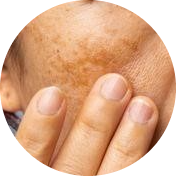
While the exact cause of melasma is still being studied, it is clear that there are several factors that contribute to the development of this condition. Understanding these factors can help individuals take steps to prevent the development of melasma or manage the condition if it does occur.
Melasma During Pregnancy
Melasma during pregnancy, also known as chloasma gravidarum, is a common occurrence that affects many women. It is estimated that up to 50-70% of pregnant women will experience some degree of hyperpigmentation on their skin, with melasma being one of the most common forms. The exact cause of melasma during pregnancy is not fully understood, but it is believed to be related to the hormonal changes that occur during gestation. Specifically, increased levels of estrogen and progesterone may stimulate the production of melanin, leading to hyperpigmentation on the skin.
The prevalence of melasma during pregnancy is influenced by several factors, including:
- Age
- Skin color
- Sun exposure
Women who are older, have darker skin tones, or live in regions with high levels of UV radiation are more likely to develop melasma during pregnancy. Additionally, women who have a family history of melasma or have previously experienced the condition are at an increased risk of developing it during pregnancy.
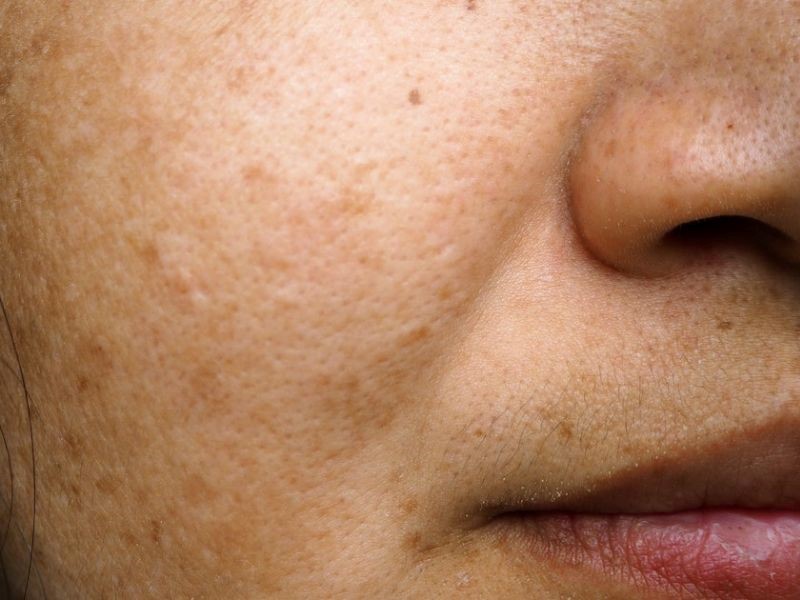
Melasma during pregnancy typically presents as dark patches on the face, including the forehead, cheeks, and upper lip. The patches may be symmetrical and may increase in size and intensity as the pregnancy progresses. While the condition is not harmful to the mother or the developing fetus, it can be distressing for many women and may impact their self-esteem and quality of life. Some studies have suggested that women who experience melasma during pregnancy may be more likely to experience postpartum depression, highlighting the need for appropriate management and support for affected individuals.
Management of melasma during pregnancy is challenging, as many traditional treatment options are not recommended during gestation. Sun protection, including the use of broad-spectrum sunscreen and protective clothing, is essential in preventing the development and worsening of melasma during pregnancy. Topical treatments such as hydroquinone and retinoids should be avoided during pregnancy, as they may be harmful to the developing fetus. In some cases, laser or light therapies may be considered after delivery, but these should only be performed under the guidance of a qualified skin dermatologist. Overall, the best approach to managing melasma during pregnancy is prevention through sun protection and avoidance of known triggers, coupled with appropriate support and counseling for affected individuals.

Melasma Mustache
Melasma Mustache is a type of hyperpigmentation that causes dark patches of skin to appear on the upper lip area, resembling a mustache. It is a common condition that primarily affects women and is caused by the overproduction of melanin, the pigment that gives color to the skin.
Melasma on Face
Melasma on the face is a common presentation of this condition and can be a significant source of distress for affected individuals. The patches of hyperpigmentation typically appear on the cheeks, forehead, and upper lip and can range in color from light brown to dark brown. Melasma on the face is more common in women, particularly during pregnancy, although men can also be affected. The condition can be chronic and recurrent, with patches often returning even after successful treatment, underscoring the importance of ongoing prevention and management strategies.
Melasma Treatment
Melasma treatment can be challenging as it often requires a tailored approach for each individual’s specific needs. There is no one-size-fits-all solution for melasma treatment, and what works for one person may not work for another. However, there are various treatment options available that can help improve the appearance of melasma, including:
- Chemical Peels: This process involves the application of a chemical solution on the skin, which exfoliates the top layer of the skin, revealing a new layer of skin that is less pigmented. This treatment can be effective for managing melasma, but it may require multiple sessions and may have side effects, such as redness or peeling of the skin.
- Laser Therapy: This melasma treatment takes advantage of laser technology to target the melanin in the skin, breaking it down and reducing its appearance. This treatment can be effective, but it may require several sessions and may have side effects, such as skin irritation or redness.
- Microdermabrasion: A special device is used to exfoliate the top layer of the skin, reducing the appearance of dark patches on the skin. This treatment can be effective, but it may require multiple sessions and may have side effects, such as redness or peeling of the skin.
- Sun Protection: Protecting the skin from the sun is crucial in managing melasma. Wearing broad-spectrum sunscreen with an SPF of 30 or higher and avoiding direct sunlight during peak hours can help prevent the condition from worsening.
- Topical Medications (Melasma Cream): There are several types of melasma cream available on the market, but it’s important to choose a product that is safe and effective. Some of the most commonly used melasma creams include:
- Hydroquinone: Hydroquinone is a skin-lightening agent that works by reducing the production of melanin in the skin. It is available in over-the-counter and prescription strengths.
- Tretinoin: Tretinoin is a vitamin A derivative that can improve the appearance of melasma by increasing cell turnover and reducing the production of melanin in the skin.
- Azelaic acid: Azelaic acid is a natural acid that can reduce the production of melanin in the skin and improve the appearance of dark patches caused by melasma.
These medications work by inhibiting the production of melanin, reducing the appearance of dark patches on the skin. However, these medications may take several weeks to show results, and they may have side effects, such as skin irritation or redness.

It’s important to note that some melasma creams can be irritating to the skin, so it’s essential to follow the instructions carefully and avoid using them on sensitive skin.
Managing Hyperpigmentation with Expert Dermatology Care
If you’re dealing with persistent dark patches on your skin, particularly on the face, it’s vital to seek professional guidance from our experienced hyperpigmentation dermatology specialists at RemoteDerm. These specialists can accurately diagnose melasma and recommend appropriate treatments. Don’t let your skin condition affect your confidence; take the first step towards effective management by getting an online consultation today.
Melasma Prevention
Melasma prevention is a crucial aspect of managing this condition, especially for individuals who are at higher risk of developing melasma, such as those with a family history of melasma or those with darker skin tones. Some effective strategies for preventing melasma include:
- Sun protection: Sun exposure is a known trigger for melasma, and wearing protective clothing and using a broad-spectrum sunscreen with an SPF of at least 30 can help prevent the development and worsening of the condition.
- Hormone regulation: certain medications, such as birth control pills and hormone replacement therapy, can trigger the development of melasma. Talk to your healthcare provider about alternative options if you are at risk of developing melasma.
- Skincare: avoiding certain skincare products, such as those containing fragrances or essential oils, can help prevent melasma. Additionally, gentle exfoliation and hydration can help improve the appearance of existing melasma and prevent the development of new patches.
- Dietary changes: Some studies suggest that dietary factors, such as antioxidant-rich foods and certain supplements, may help prevent the development of melasma. However, more research is needed in this area.

In addition to these prevention strategies, it is important for individuals at risk of developing melasma to be vigilant about changes in their skin and to seek medical advice if they notice any unusual patches or discoloration. Early intervention and treatment can help prevent the condition from worsening and can improve the overall prognosis for affected individuals. Dermatologists can work with their patients to develop personalized prevention plans that take into account their individual risk factors and preferences.
Conclusion
Melasma is a common skin condition that can be distressing for those who experience it. While the exact cause of melasma is not fully understood, it is known to be associated with hormonal changes, sun exposure, genetic predisposition, skin irritation, and certain medications. The condition is more prevalent in women, particularly during pregnancy, and those with darker skin tones.

Prevention is essential in managing melasma, and this can be achieved through the use of broad-spectrum sunscreen, protective clothing, and avoiding known triggers. Topical treatments such as hydroquinone and retinoids are not recommended during pregnancy as they can be harmful to the developing fetus. Remotederm offers patients the opportunity for an online dermatology consultation session from the comfort of their own homes, making it easier to manage the condition.
While melasma can be challenging to manage, ongoing prevention and management strategies can help individuals achieve the best possible outcomes. For those experiencing distress related to melasma, appropriate support, and counseling can be beneficial. Overall, with appropriate care and support, individuals with melasma can maintain good skin health and enjoy a good quality of life.
FAQs
1. Is Melasma contagious?
No, Melasma is not contagious. It is a non-infectious skin condition and cannot be passed from one person to another.
2. Can Melasma be treated with over-the-counter remedies?
Over-the-counter remedies may help improve the appearance of melasma, but they are unlikely to completely remove it. It’s best to consult a dermatologist for a personalized treatment plan.
3. Can birth control pills cause Melasma?
Yes, birth control pills can trigger melasma in some women due to the hormonal changes they cause. Other factors such as pregnancy and sun exposure can also contribute to the development of melasma.
4. Is it possible for Melasma to go away on its own?
Melasma can fade on its own, but it may take several months or even years. To speed up the process, it’s important to protect your skin from sun exposure and follow a recommended treatment plan.
5. What are some natural remedies for melasma?
While there’s no single natural remedy that works for everyone, some people have found success using a combination of ingredients like turmeric, apple cider vinegar, and lemon juice. It’s important to note, however, that natural remedies should be used with caution and ONLY under the guidance of a healthcare professional.
6. Can melasma be cured completely?
Unfortunately, there’s no cure for melasma, but it can be managed with a combination of treatment methods and lifestyle changes. With proper care, many people with melasma see a significant improvement in the appearance of their skin.

2 comments
I have melasma on my upper lip and it looks like a mustache. I hate it so much. How can I get rid of it fast?
We’re sorry to hear that you’re unhappy with your melasma. Unfortunately, there is no quick fix for this condition, as it may take several months or even years to fade. However, you can try some treatments that may help lighten your melasma, such as skin lightening creams, chemical peels or laser therapy.