Hormonal acne, characterized by persistent breakouts influenced by hormonal fluctuations, poses a unique challenge for many individuals, including Canadians. While it can be a source of frustration, understanding the causes and adopting targeted treatment strategies can significantly improve the complexion and boost confidence. In this comprehensive guide, we’ll delve into the intricate details of hormonal acne, explore its underlying causes, and provide in-depth insights into proven treatment methods.
Understanding Hormonal Acne
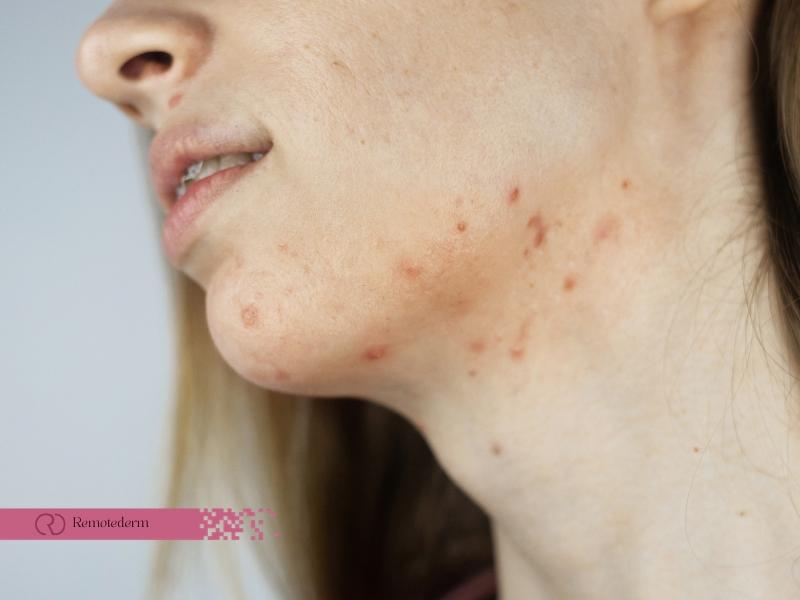
Hormonal acne is closely tied to the body’s hormonal fluctuations, specifically androgens, which stimulate the sebaceous glands. This stimulation results in an overproduction of sebum, leading to clogged pores and subsequent acne breakouts. Regions commonly affected by hormonal acne include the chin, jawline, and lower face. Recognizing these patterns is essential for tailoring an effective treatment plan. By understanding the connection between hormonal imbalances and acne, individuals can adopt targeted strategies to manage breakouts and achieve clearer, healthier skin. Seeking guidance from a dermatologist, whether in-person or through an online acne dermatologist, further enhances the ability to navigate and address the complexities of hormonal acne with personalized insights and professional support.
Causes of Hormonal Acne
Hormonal acne, a skin condition characterized by persistent breakouts, is intricately tied to hormonal fluctuations within the body. Several factors contribute to the development of hormonal acne, shedding light on its complex nature:
- Puberty: Adolescence initiates hormonal changes, particularly an increase in androgen levels. This surge in hormones stimulates the sebaceous glands, leading to heightened sebum production and increased susceptibility to acne.
- Menstrual Cycle: Women often experience hormonal fluctuations during their menstrual cycle. The premenstrual phase, characterized by elevated androgen levels, can result in the development of acne, especially along the jawline and chin.
- Pregnancy: Pregnancy induces significant hormonal shifts, impacting the skin’s oil production. While some women may experience clearer skin during pregnancy, others may contend with hormonal acne as a result of these fluctuations.
- Polycystic Ovary Syndrome (PCOS): PCOS is a hormonal disorder affecting women of reproductive age. It leads to an imbalance in androgen levels, contributing to acne development. Individuals with PCOS often experience persistent and widespread acne.
- Hormonal Medications: Certain hormonal medications, including contraceptives and hormone replacement therapy, can influence sebum production, potentially causing or exacerbating acne.

Hormonal Acne Treatment Strategies
Effectively managing hormonal acne demands a multifaceted approach that addresses the intricate interplay of hormones and skin health, something many Canadians can relate to. The following treatment strategies offer a comprehensive solution to the challenges posed by hormonal acne:
- Topical Treatments
Embrace the power of topical solutions enriched with active ingredients like benzoyl peroxide, salicylic acid, or retinoids. These compounds play a crucial role in unclogging pores, diminishing inflammation, and thwarting the progression of further breakouts. By directly targeting affected areas, these topicals offer a localized yet potent defense against hormonal acne.
- Oral Medications
For cases requiring internal intervention, dermatologists may recommend oral contraceptives or anti-androgen medications. These medications serve to regulate hormonal imbalances and exert control over acne development. Additionally, antibiotics may be prescribed to tackle inflammatory responses and combat bacteria contributing to acne formation. This systemic approach ensures a holistic influence on hormonal factors affecting the skin.
- Skincare Routine
Establishing a consistent and tailored skincare routine forms the foundation of hormonal acne management. Gentle cleansers help maintain a balanced complexion, non-comedogenic moisturizers prevent excessive oiliness, and sunscreen safeguards against potential aggravators. This routine not only fosters skin health but also mitigates the risk of irritation, a key consideration for those combating hormonal acne.

- Lifestyle Adjustments
Recognizing the profound impact of lifestyle on hormonal balance, individuals can implement strategic adjustments. Stress, a known trigger for hormonal fluctuations, can be managed through practices like meditation or yoga. Regular exercise contributes to overall well-being, while maintaining a nutrient-rich, balanced diet supports hormonal equilibrium. These lifestyle modifications synergize with other treatment approaches to fortify the body’s resilience against hormonal acne.
- Dietary Considerations
Explore the correlation between diet and hormonal acne by evaluating specific dietary choices. Some individuals find that minimizing dairy or reducing refined sugars positively influences their skin health. Consulting with a healthcare professional or dermatologist is essential for personalized dietary advice, ensuring that nutritional adjustments align with individual needs and contribute to long-term acne management.
In combining these nuanced strategies, individuals can customize their approach to address the unique triggers of hormonal acne. Consulting with a dermatologist, whether in-person or through an online acne dermatologist, is crucial.
Their expertise enables personalized guidance and targeted treatment plans for lasting clarity and vibrant skin. The accessibility of online consultations enhances convenience, providing flexibility and expert support on the journey to healthier, acne-free skin. This amalgamation of tailored strategies and expert consultation forms a powerful and holistic approach to managing hormonal acne effectively.
Final Thoughts
In conclusion, addressing the challenges of hormonal acne requires a comprehensive and personalized approach, one that resonates with many Canadians. This guide has provided insights into the diverse causes of hormonal acne, ranging from puberty-related hormonal shifts to the influences of the menstrual cycle, pregnancy, PCOS, and hormonal medications. The outlined treatment strategies offer a roadmap for those seeking enduring clarity and vibrant skin, encompassing topical treatments, oral medications, a meticulous skincare routine, lifestyle adjustments, and dietary considerations. Each facet of this multifaceted approach contributes to a holistic solution tailored to the unique triggers of hormonal acne.
Consultation with a dermatologist, whether through traditional in-person visits or the convenience of an online acne dermatologist, remains pivotal. Their expertise enables personalized guidance and the formulation of targeted treatment plans. The accessibility of online consultations adds a layer of convenience, allowing individuals in Canada and beyond to navigate their path to healthier, acne-free skin with flexibility and expert support. By amalgamating these nuanced strategies and leveraging professional consultation, individuals embark on a powerful journey to effectively manage hormonal acne. Through this collaborative effort, lasting clarity and skin vibrancy become tangible goals, marking the end of the frustrating battle with hormonal acne and the beginning of a confident and revitalized skincare journey.
FAQs
- How is hormonal acne different from other types of acne?
Hormonal acne is distinguished by its correlation with hormonal fluctuations, often appearing along the chin, jawline, and lower face, whereas other types of acne may result from different factors like bacteria or clogged pores.
- Can pregnancy cause hormonal acne?
Yes, pregnancy induces significant hormonal shifts that can impact oil production, leading to hormonal acne in some women.
- How long does it take for hormonal acne treatments to take effect?
The timeline for improvement varies, but individuals may start seeing results within a few weeks to a couple of months, depending on the treatment method.
- Can hormonal acne be completely cured, or is it a lifelong condition?
While it can be effectively managed, hormonal acne may require ongoing maintenance, as hormonal fluctuations continue throughout life.