Acne is a skin condition that occurs when the pores in the skin become clogged with oil and dead skin cells. It is a common condition that affects a significant portion of the global population, with estimates suggesting that it affects around 9.4% of people worldwide. In the United States, acne is the most common skin condition, according to the American Academy of Dermatology.
Although acne is generally not a serious health threat, it can cause discomfort and pain, especially when it is severe. Over time, untreated or improperly treated acne can also lead to scarring.
This post will provide a detailed overview of the various types of acne, their symptoms, diagnostic methods, acne treatment options, and prevention strategies.
Overview
Acne vulgaris is a common cutaneous disorder that can cause pain and disfigurement and have a negative psychosocial impact. Acne vulgaris clinical manifestations range from minor skin involvement to severe manifestations.

Acne vulgaris can be treated with topical, oral, and procedural therapies. Although topical therapy is the primary treatment option for mild acne vulgaris, patients with moderate to severe manifestations may benefit from systemic therapy. Systemic therapy for acne vulgaris includes antibiotics, isotretinoin (Accutane), and hormonal agents.
Epidemiology of Acne
Acne vulgaris is most commonly seen in adolescents and young adults. Prevalence estimates for teenagers with acne vulgaris range from 35% to over 90%. Acne may begin in preadolescent years (ages 7-12) and resolve in the third decade, but it can also persist into adulthood or even appear for the first time in adulthood. In general, males are more likely to experience adolescent acne than females, but postadolescent acne affects more women than men.
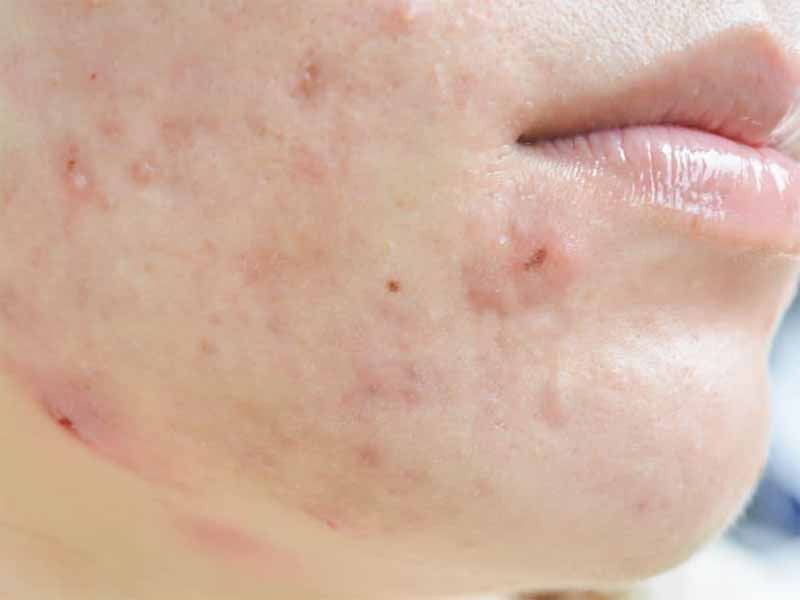
As people age, the incidence of acne tends to decrease. A study of over 1000 adults in the United States found the following self-reported rates of acne in males and females:
- 20 to 29 years—43 and 51%, respectively.
- 30 to 39 years—20 and 35%, respectively.
- 40 to 49 years—12 and 26%, respectively.
- Ages 50 and older: 7 and 15%, respectively.
There is often a discrepancy in the prevalence of acne reported in surveys based on self-reported symptoms compared to those identified through clinical examinations. Infantile acne, a form of acne vulgaris, may occur in children, but mid-childhood acne (occurring between the ages of one and six) is rare and may signal the presence of an underlying health issue that requires further examination.
We suggest you to read another article about skin dermatologist in Remotederm by click on the link.
Different types of Acne
Although the term “breakout” is often used to refer to all forms of acne, this is not always a precise description. Acne can present in various ways and is caused by blockages in the pores. These blockages can be caused by a range of factors, including:
- Excess oil production (sebum)
- Bacteria
- Hormones
- Discarded skin cells
- Ingrown hair
Acne is not only a common issue during adolescence, as it can also affect adults. In fact, about 17 million Americans have acne, making it one of the most common skin conditions among both children and adults. If you have acne, you may experience various types of pimples. It is important to correctly identify the type of acne you have in order to effectively treat it. Whiteheads and blackheads, also known as comedones, are the most common types of acne lesions.
-
- Blackheads, also called open comedones, are visible on the surface of the skin and appear dark due to oxidation, not dirt. These skin pimples, which are open comedones visible on your skin, get their darker color from the oxygen in the air.
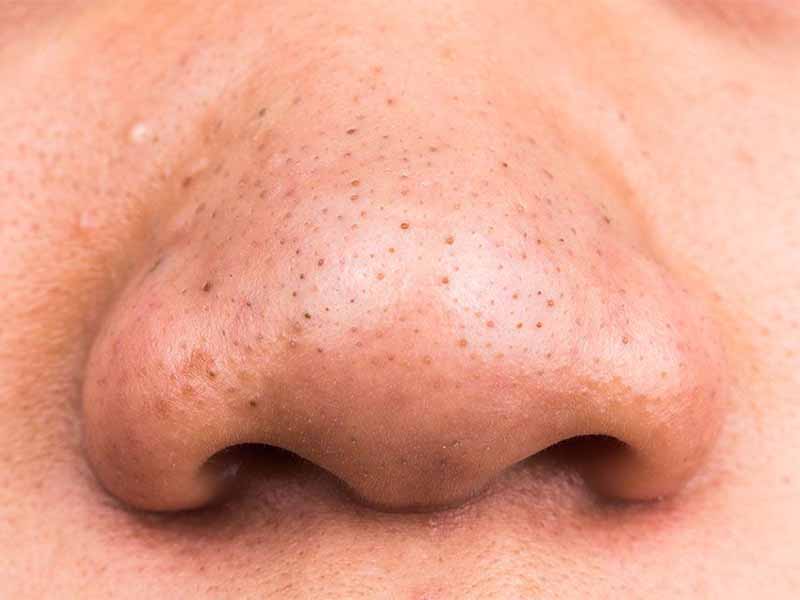
- Whiteheads, or closed comedones, appear as raised bumps beneath the surface of your skin. They remain flesh-colored.
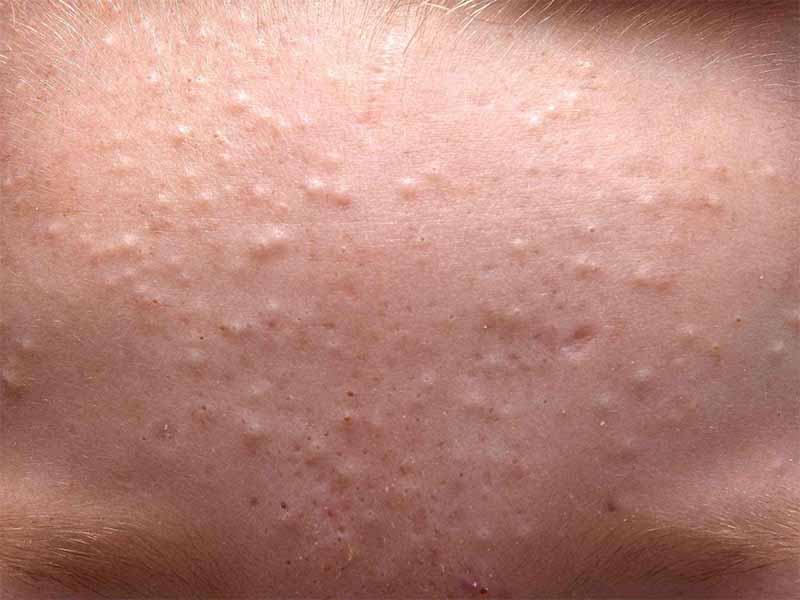
The following inflammatory lesions are more likely to result in skin scarring:
- Papules. Hair follicles that are inflamed or infected cause these small, red, raised bumps.
- Pustules. The tips of these small red pimples are filled with pus.
- Nodules. These solid, often painful lumps form beneath the surface of your skin.
- Cysts. These big bumps under your skin usually hurt and are filled with pus.
- Fungal acne (Pityrosporum folliculitis): This type develops when there is an overabundance of yeast in the hair follicles. They might become swollen and itchy.
Any type of acne can potentially have an impact on a person’s self-esteem, and it is important to consult with a healthcare provider as soon as possible to determine the best treatment option(s). Your healthcare provider can help you choose the best course of action to manage your acne.
What causes Acne?
Acne vulgaris is a skin condition that affects the pilosebaceous unit, which includes the hair follicle and the sebaceous gland that produces sebum, or natural skin oil. It commonly appears on the face, forehead, chest, upper back, and shoulders due to the high concentration of oil glands in these areas.
When the walls of hair follicles become inflamed, whiteheads may form. Blackheads, on the other hand, occur when a plug is exposed to the surface and darkens due to the oxidation of bacteria and oil when in contact with air.
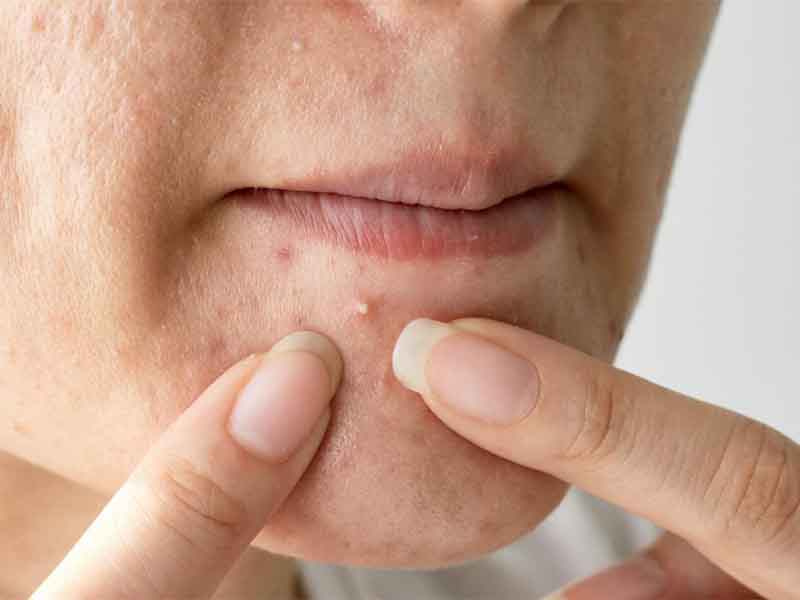
Skin pimples are raised red spots with a white center that occur when hair follicles become inflamed or infected with bacteria. Cyst-like lumps may also form under the skin’s surface due to blockages and inflammation within the hair follicles. Acne rarely affects other skin pores, which are the openings to sweat glands.
Acne can be caused or aggravated by certain factors:
- Hormonal changes. Androgens are a type of hormone that increase in levels during puberty in both males and females. This increase in androgens causes the sebaceous glands to grow and produce more sebum, which can lead to breakouts. Hormonal changes in midlife, particularly in women, can also contribute to the development of acne.
- Certain medications. Corticosteroids, testosterone, and lithium-containing medications are a few examples.
Curious about ‘Can antibiotics cause acne’? Check out our article for the answer!
- Diet. Certain foods have been shown in studies to aggravate acne, including skim milk & carbohydrate-rich foods like bread and potato chips. More research is needed, however, to determine whether certain dietary restrictions would benefit acne patients.
- Stress. Although stress does not cause acne, it can aggravate it if you already have it.
Diagnosis of Acne
Acne can be diagnosed by a healthcare provider during a skin examination. They may ask about your stress levels and family history of acne, as well as association with your menstrual cycles in teenage girls and women, as these can be risk factors for breakouts. In older individuals, sudden and severe acne outbreaks may be a sign of an underlying medical condition that requires treatment. The type and location of treatment for acne will depend on its severity.
It is important to note that what appears to be acne may actually be another skin condition, such as acne inversa (also known as hidradenitis suppurativa) or perioral dermatitis. These conditions may cause breakouts that resemble acne but require different treatment. If you have persistent acne or suspect you may have another skin condition, it may be helpful to consult with a board-certified dermatologist for a proper diagnosis and customized treatment plan.
Signs and Symptoms of Acne
Acne commonly appears on the face and shoulders. It may also occur on the trunk, arms, legs, and buttocks. The appearance of acne can vary from person to person; however, common skin changes include:
- Skin bumps with crusting
- Cysts
- Papules (small red bumps)
- Pustules (small, red bumps with white or yellow pus)
- Redness around skin eruptions
- Skin Scarring
- Whiteheads
- Blackheads
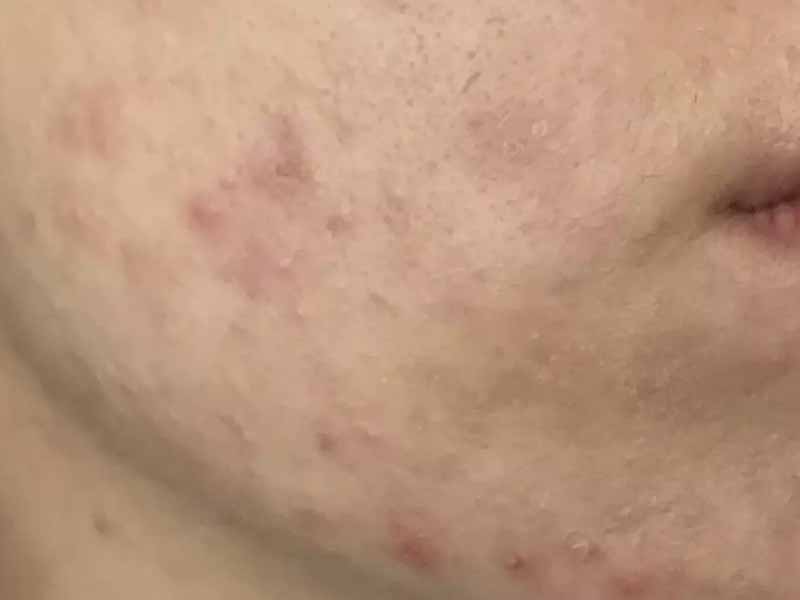
Classic Acne features
As mentioned earlier, acne vulgaris is most commonly found in areas of the body with large, hormonally responsive sebaceous glands, such as the face, neck, chest, upper back (Bacne), and upper arms. There may be one or more types of active lesions present, such as:
- Closed comedones are smooth, dome-shaped, less than 5 mm in diameter, non-inflammatory, and skin-colored, whitish or grayish papules.
- Open comedones are non-inflamed papules with less than 5 mm in diameter that have a central, dilated follicular orifice that is filled with gray, brown, or black keratotic material.
- Papulopustular acne is distinguished by inflamed, relatively superficial papules and pustules 5 mm in diameter.
- Deeply seated, inflamed, frequently tender, large papules (bigger than 0.5 cm) or nodules, which characterize nodular acne (bigger than 1 cm),
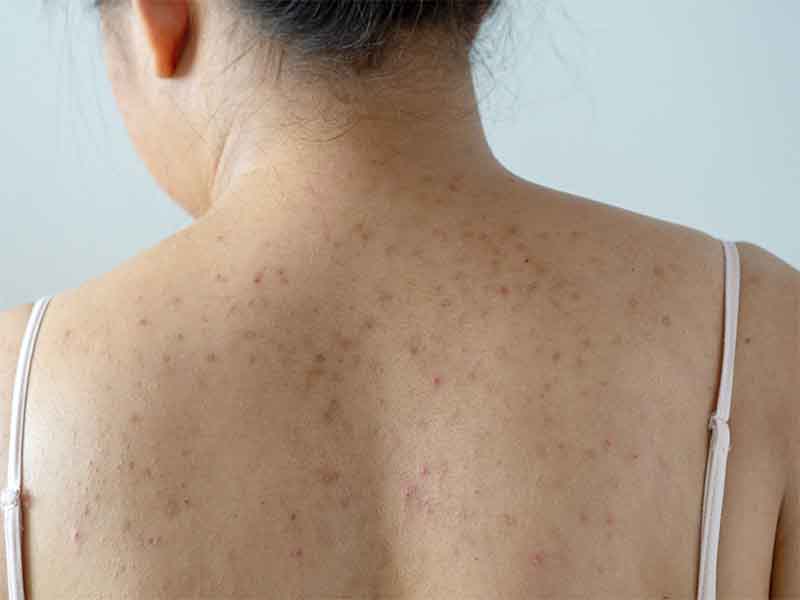
Acne with nodules is occasionally incorrectly referred to as “cystic” or “nodulocystic” acne. True cysts are actually quite uncommon.
In patients with highly pigmented skin, skin pigmentation may conceal the distinctive erythema of inflamed lesions.
The extent and severity of skin involvement varies greatly, from the appearance of a few small comedones on a regular basis to the chronic presence of numerous inflamed nodules involving the majority of skin in an affected region.
Acne Treatment options
Acne vulgaris is a common skin condition that ranges from mild to severe. There are various treatment options available, including topical and systemic therapies. Topical medications, such as retinoids, benzoyl peroxide, and antibiotics, are applied directly to the skin and can help reduce the formation of comedones (clogged pores). Systemic medications, such as oral contraceptives and spironolactone, work by targeting the underlying cause of acne, which may include hormonal imbalances or excess oil production. Procedures, such as chemical peels or laser treatments, may also be used in conjunction with other therapies to help improve the appearance of the skin.

It is important to work with a dermatologist or healthcare provider to determine the best treatment plan for your individual needs and skin type.
When to use systemic therapy?
Moderate to severe acne vulgaris is often treated with systemic therapy in order to improve and simplify treatment. The main systemic treatments for acne vulgaris are oral antibiotics (usually tetracyclines), hormonal treatments (oral contraceptives or spironolactone), and oral isotretinoin.

Systemic therapy is usually used in combination with topical therapy, with the exception of oral isotretinoin. The decision to start systemic therapy is influenced by the patient’s clinical presentation and preferences. Clinical findings such as nodular lesions, widespread skin involvement, scarring, and psychological distress related to acne may indicate the need for systemic therapy. If these findings are not present, it is reasonable to try topical therapy first; however, dermatologists usually discuss the option of systemic therapy with all patients with moderate to severe acne vulgaris.
Choosing a systemic Acne treatment
The selection of systemic treatments (oral isotretinoin, oral antibiotics, and oral hormonal agents) requires consideration of patient-specific characteristics as well as individual patients’ values and preferences.
- Symptoms: The type of lesions present, as well as the severity of acne vulgaris, influence therapy selection:
- Types of lesions
- Severity
- Sex and age: Systemic hormonal therapy (oral contraceptives, spironolactone) is mostly available to postmenopausal female patients with acne vulgaris.
- Pregnancy and childbearing potential: Certain systemic therapies are not advised to be used while pregnant. Pregnant women should not take oral isotretinoin, oral tetracyclines, oral contraceptives, or spironolactone.
When to use topical therapy?
Combining different types of treatment, such as topical and systemic therapy, is often recommended for patients with acne vulgaris to maximize their response to treatment. However, oral isotretinoin is usually administered as a single treatment.

For patients who prefer not to receive systemic therapy, combining different skin-directed therapies is often an option. Different treatments are used to target the various causes of acne vulgaris, and treatments with different mechanisms of action, such as topical antibiotics, topical retinoids, salicylic acid, and azelaic acid, can be included.
For mild acne vulgaris, a minimal approach using topical therapy, such as a retinoid and benzoyl peroxide, may be recommended for patients with comedonal acne.
Common topical acne treatments include:
- Salicylic acid is a cleanser or lotion that is sold over-the-counter to treat acne.It helps to remove the damaged top layer of skin. Salicylic acid removes dead skin cells, preventing hair follicles from clogging.
- Azelaic acid is a natural acid that can be found in many grains, including rye, barley, and wheat. It lessens swelling while also eradicating skin-surface microorganisms.
- Antibiotics (topical types include clindamycin and erythromycin) inhibit surface bacteria that aggravate and frequently promote acne swelling. When antibiotics are combined with benzoyl peroxide, they are more effective.
- Dapzone (Aczone®) is a topical gel with antibacterial properties that can be used to treat inflamed acne. It is applied twice daily to the skin.
- Retinoids (vitamin A derivatives) Retin-A®, Tazorac®, and Differin® (which is now available without a prescription) break up blackheads and whiteheads and help to prevent clogged pores, the first signs of acne. The majority of patients are candidates for retinoid therapy. These medications are not spot treatments and must be applied to the entire area of skin affected by acne to prevent the formation of new comedones. Irritation is the most typical side effect, and it typically goes away with time and use of the drug.
- Benzoyl peroxide is a leave-on gel or wash that is sold over-the-counter under the brand names Clearasil, Stridex, and PanOxyl. It targets the surface bacteria that regularly exacerbates acne. Your skin won’t be as irritated by wash formulations and lower concentrations. One typical side effect is irritation (dryness).
Patients may also benefit from the incorporation of procedural therapies, such as chemical peels or laser therapy.
Oral medications (those taken by mouth):
- Antibiotics, Tetracycline antibiotics, particularly minocycline and doxycycline, are frequently used to treat moderate to severe acne.
- Oral contraceptives can aid in the treatment of menstrual cycle-related breakouts. For people with acne, the FDA has approved three different classes of drugs. Estrostep®, Beyaz®, Ortho Tri-Cyclen®, and Yaz® are a few examples of brand names.
- Isotretinoin An oral retinoid (Amnesteem®, Claravis®, Sotret®) is a highly effective medication reserved for the most severe cases of acne. Oil gland size decreases caused by isotretinoin contribute to acne development. Dryness is the most frequent adverse effect, but it can also result in birth defects. There is some evidence that depression and ulcerative colitis may be more common.
Looking for specialized expertise? Consider consulting an acne dermatologist to guide you through effective treatment options. These experts are trained to diagnose the root causes of acne and tailor treatment plans to your individual needs.
How to prevent Acne?
There are ways to help prevent new acne spots from appearing and acne scars from forming if you have acne. The following will help keep spots from becoming inflamed or scarred:
- Use a mild soap-free wash, warm water, and a soft face cloth to wash your face twice daily.
- When you are outside in the sun, protect your skin by wearing a wide-brimmed hat and sunscreen.
- Before going to bed, remove your makeup.
- Regularly shampoo your hair, particularly if it is oily and lays on your skin.
- Maintain a balanced, healthy diet and engage in regular physical activity
Avoid the following:
- Greasy sunscreen or oil-based makeup
- Using abrasive soaps or frequently washing your face
- Using facial cleansers, toners, or scrubs too often
- Tight clothing over acne-prone areas
- Squeezing or picking at pimples or spots
- Smoking

Acne most commonly affects people between the ages of 15 and 24, and many people notice fewer and less severe spots by their mid-twenties. Some people, on the other hand, do not grow out of acne and will require ongoing treatment.
Acne also affects people with naturally oily skin. While you cannot change your age or skin type, knowing that there are methods for managing acne and caring for your skin can be helpful.
Bottom Line
Acne can be difficult to treat, but there are many effective treatments available to help reduce breakouts and heal your skin. Different types of acne require different treatments, and sometimes a combination of methods is required.

Consult a dermatologist for treatment options if you notice any acne symptoms or reddish sensitive bumps. If your schedule prevents you from visiting a clinic in person, you can always benefit from an online dermatologist appointment in Canada. An online dermatologist appointment can be a convenient and secure way to get the treatment you require without leaving the comfort of your own home.
You can get more information about online dermatology consultation by click on the link.
Acne FAQs
1. If I have Acne, should I stop wearing makeup?
You don’t have to stop wearing makeup entirely, but you could experiment with different brands or types. According to dermatologists, if you have breakouts along the sides of your temples, hair creams or gels may be exacerbating your acne. Look for cosmetics and toiletries labeled “non-comedogenic,” which means they don’t clog pores.
2. Is Acne a sign that I’m not washing my face properly?
No, not always. Scrubbing your face too hard can aggravate acne, and using alcohol-based astringents can dry out your skin. Hormones cause acne, and while gentle, regular cleansing with soap and warm water can sometimes help with mild breakouts, more severe acne necessitates more than just good hygiene.
3. How do I treat Acne on dark skin?
Acne and dark spots can be treated at the same time. Acne scars on dark skin are more likely to form pigmentary scars. Retinol and benzoyl peroxide can be used to treat mild acne. Cocoa butter, shea butter, and coconut oil should not be used on the face because they will clog pores. Use non-comedogenic products and a gentle cleanser containing salicylic or glycolic acid.
4. Why is picking or squeezing Acne spots harmful?
The issue with this is that it can push the inflamed spot deeper into the skin, causing damage to healthy skin tissue. This increases the risk of spreading the infection as well as the acne outbreak, and it may result in scarring. It is tempting to do so, but resist the urge.
5. How do Acne scars develop?
These are typically caused by severe acne or squeezing pimples. Acne that is severe manifests as a series of pus-filled sores that can spread and damage the surrounding skin. Scarring is the end result of this. Picking or squeezing the affected area will also result in a scar.
6. Is chocolate consumption a cause of Acne?
Despite decades of research, there is little evidence that single foods like chocolate cause acne. But that doesn’t mean diet has no effect. The sugar in your chocolate bar or cupcake is more likely to be to blame for new pimples or deeper breakouts than the cocoa itself.
7. Will my Acne ever clear up?
Although acne typically disappears on its own at the end of puberty, some people continue to experience acne as adults. But almost all cases of acne can be effectively treated. It all comes down to getting the right treatment for you.

10 comments
I liked the info provided by this article!however I was wondering if there are any natural remedies that can be effective for treating acne?
We appreciate your feedback! While there are some natural remedies that may help alleviate acne symptoms, such as tea tree oil or aloe vera, it’s important to remember that they may not be as effective as clinically proven treatments. We recommend consulting with a dermatologist to determine the best treatment plan for your individual needs.
I found the section on different types of acne very informative. Can you provide more information on how to differentiate between different types of acne?
We’re glad you found that section helpful! Different types of acne can vary in appearance and severity. Some types include whiteheads, blackheads, papules, pustules, cysts, and nodules. A dermatologist can help diagnose your specific type of acne based on its appearance and recommend an appropriate treatment plan.
Are there any effective treatments for reducing the appearance of acne scars?
Treatment options for reducing the appearance of acne scars include chemical peels, microdermabrasion, laser therapy, and dermal fillers. A dermatologist can help determine the best treatment plan for your individual needs.
Are there any specific skincare products that are recommended by dermatologists for preventing acne?
It’s important to choose skincare products that are labeled as “non-comedogenic” or “oil-free” and to avoid using products that contain ingredients that can clog pores, such as cocoa butter or coconut oil. A dermatologist can also recommend specific products that are tailored to your individual needs.
I’ve heard mixed opinions about whether diet affects acne. Can you provide more information on the link between diet and acne, and if there are specific foods to avoid or incorporate into the diet?
Ongoing research suggests diet affects acne; high-glycemic foods and dairy could play a role. Including fruits, vegetables, and a balanced diet can help. For more on this, check our blog’s Acne category. Consulting a healthcare professional for personalized advice is recommended.