Comedonal acne is a common skin condition characterized by small, flesh-colored or white bumps that appear on the face, forehead, chin, and nose. These bumps, also known as comedones, occur when the hair follicles become clogged with oil and dead skin cells. Comedonal acne is not painful, but it can be frustrating and difficult to treat. In this article, we will discuss dermatologist-approved treatments and skincare tips that can help you win the battle against comedonal acne.
What are Comedones?
Comedonal acne is a common skin condition that is caused by the accumulation of oil and dead skin cells in hair follicles. Open and closed comedones are the two different types.
- Open comedones, also known as blackheads, occur when the clogged hair follicle is open to the skin’s surface. The contents of the pore oxidize, resulting in the characteristic black color. Blackheads can be unsightly and can lead to larger acne lesions if not properly treated.
- Closed comedones, on the other hand, occur when the clogged hair follicle remains closed and appears as a small, flesh-colored bump on the skin’s surface. These bumps are often difficult to treat, as they do not have an opening to the surface of the skin.
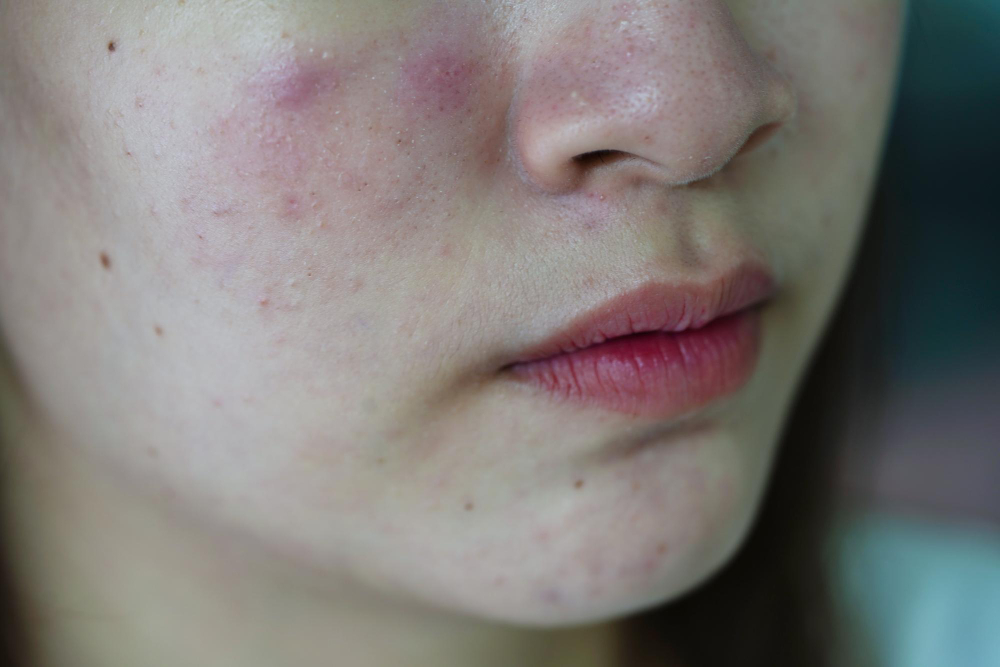
If you are struggling with comedonal acne, don’t worry. There are a variety of dermatologist-approved treatments and skincare tips available to help manage and prevent its formation. Don’t let acne control your life, learn how to prevent outbreaks and scarring with expert tips from our dermatologists at RemoteDerm.
Comedonal Acne Causes
While it is important to focus on finding the right treatment to manage comedonal acne, it is also important to understand the underlying causes of this condition. Here are some of the most common comedonal acne causes:
- Excess sebum production: Comedonal acne is often caused by excess sebum, or oil, production. This can lead to clogged pores and the formation of comedones.
- Poor skin cell turnover: When skin cells do not shed properly, they can accumulate and mix with sebum to create a plug in the hair follicle.The outcome of this can be the development of comedones.
- Hormonal changes: Hormonal changes can play a role in the development of comedonal acne. Hormonal fluctuations, such as those that occur during puberty or the menstrual cycle, can increase sebum production and contribute to the formation of comedones.
- Certain medications: Some medications, such as steroids or birth control pills, can contribute to the development of comedonal acne.
- Genetics: Like many skin conditions, genetics can play a role in the development of comedonal acne. If you have a family history of acne, you may be more prone to developing comedones.

Understanding the causes of comedonal acne can help you take steps to prevent its formation. While some causes, such as genetics, cannot be controlled, focusing on a good skincare routine and addressing any underlying hormonal imbalances can go a long way in managing this condition.
Comedonal Acne Treatment Recommended by Dermatologists
When it comes to treating comedonal acne, there are several dermatologist-approved treatment options depending on the severity of the condition. Here are some of the top recommended treatments:
- Topical retinoids: Retinoids are derivatives of vitamin A and work by increasing skin cell turnover, which helps to unclog pores and prevent comedones from forming. Some common retinoids used to treat comedonal acne include tretinoin, adapalene, and tazarotene.
- Salicylic acid: This beta-hydroxy acid exfoliates the skin and helps to unclog pores, making it an effective treatment for comedonal acne. Salicylic acid can be found in a variety of over-the-counter products such as cleansers, toners, and spot treatments.
- Benzoyl peroxide: This ingredient helps to kill acne-causing bacteria and reduces inflammation. It can be found in both prescription and over-the-counter products, and is often used in combination with other acne treatments.
- Chemical peels: Chemical peels use acids such as glycolic acid or salicylic acid to exfoliate the skin and remove comedones. They can be done in a dermatologist’s office or with at-home kits, but it’s important to follow instructions carefully to avoid damaging the skin.
- Extraction: Dermatologists can use special tools to extract comedones from the skin. This can be an effective treatment for stubborn or deep comedones, but should only be done by a trained professional to avoid scarring or infection.
- Oral medications: In some cases, dermatologists may recommend oral medications such as antibiotics or isotretinoin to treat more severe cases of comedonal acne.

It’s important to work with a dermatologist to determine the best treatment plan for your specific case of comedonal acne. They can help you choose the most effective treatments while also minimizing potential side effects. Additionally, practicing good skincare habits such as regularly cleansing your skin and avoiding pore-clogging products can help prevent comedones from forming in the first place.
Skincare Tips for Comedonal Acne
If you’re dealing with comedonal acne, there are a few simple skincare tips that can help improve your skin’s overall health and reduce the occurrence of breakouts. Here are some recommendations from dermatologists to help you manage comedonal acne:
- Use a mild, non-comedogenic cleanser to wash your skin twice daily. This will help remove excess oil, dirt, and dead skin cells that can clog pores and lead to comedones.
- Avoid using harsh scrubs or exfoliants can cause skin irritation.. Instead, opt for chemical exfoliants such as salicylic acid or glycolic acid that can help gently unclog pores and improve skin cell turnover.
- Use non-comedogenic moisturizers to keep the skin hydrated. Moisturizing can help maintain the skin’s natural barrier and prevent excess oil production.
- Avoid picking or squeezing comedones, as this can lead to scarring and infection. Instead, consider using acne patches or spot treatments to help reduce the appearance of pimples.
- Use oil-free, non-comedogenic makeup products. Makeup can clog pores and contribute to the formation of comedones, so it’s important to choose products that won’t exacerbate the issue.
- Keep hair and hair products away from the face. Hair products can contain oils and other ingredients that can irritate the skin and contribute to breakouts. Keeping hair away from the face can help prevent this.
- Avoid touching the face throughout the day, as this can transfer bacteria and oil to the skin. This can exacerbate acne and lead to further breakouts.

By following these simple skincare tips, you can help improve the appearance of your skin and manage the occurrence of comedonal acne. If your symptoms persist, it’s always a good idea to consult with a dermatologist for additional guidance and treatment options.
Conclusion
In conclusion, comedonal acne can be frustrating and difficult to treat, but there are several dermatologist-approved treatments and skincare tips available that can help manage and prevent its formation. Understanding the underlying causes of comedonal acne, such as excess sebum production and poor skin cell turnover, can also help take preventative steps. Topical retinoids, salicylic acid, benzoyl peroxide, chemical peels, extraction, and oral medications are all effective treatments that can be recommended by dermatologists. Additionally, practicing good skincare habits such as regularly cleansing your skin and avoiding pore-clogging products can help prevent comedones from forming.

Remotederm online dermatology consultation services can be accessed from anywhere, eliminating the need for long waits to visit dermatologists in person. This platform is designed to provide convenient access to quality dermatological care for patients who may face barriers to in-person visits, such as those who live in remote areas or have mobility issues. Patients can use Remotederm to discuss their comedonal acne concerns with licensed dermatologists, receive diagnoses, and obtain treatment recommendations without leaving their homes.
FAQs
1. Is comedonal acne a serious condition?
Comedonal acne is not a serious condition, but it can be frustrating and difficult to treat. It is a common form of acne that is characterized by small, flesh-colored or white bumps on the skin.
2. Can comedonal acne be cured?
While there is no cure for comedonal acne, there are a variety of treatments available that can help manage and prevent its formation. These treatments include topical retinoids, salicylic acid, benzoyl peroxide, chemical peels, and extraction.
3. Can comedonal acne be caused by stress?
Stress can contribute to the development of acne, including comedonal acne. Stress can cause hormonal changes that lead to an increase in sebum production, which can clog pores and lead to the formation of comedones.
4. What is the difference between open and closed comedones?
Open comedones are also known as blackheads and occur when the clogged hair follicle is open to the skin’s surface. Closed comedones occur when the clogged hair follicle remains closed and appears as a small, flesh-colored bump on the skin’s surface.
5. When should I see a dermatologist for comedonal acne?
If your comedonal acne is not responding to over-the-counter treatments or is causing significant distress, it may be time to see a dermatologist. They can help determine the best treatment plan for your specific case and provide prescription medications if necessary.
