Dermatitis herpetiformis is a chronic autoimmune skin condition that affects a significant number of individuals worldwide. This article aims to provide a comprehensive understanding of dermatitis herpetiformis, including its causes, symptoms, and available treatment options. Whether you are seeking information for personal knowledge or researching potential treatment strategies, this article will equip you with valuable insights into this condition.
Understanding Dermatitis Herpetiformis
Dermatitis herpetiformis is a complex and often misunderstood skin condition that can significantly impact the lives of those affected by it. While it shares similarities with other skin conditions, such as eczema or psoriasis, dermatitis herpetiformis has distinct characteristics and underlying causes that set it apart. By delving into the intricacies of this condition, we can gain a deeper understanding of its symptoms, triggers, and the various treatment options available. Let’s explore the world of dermatitis herpetiformis and shed light on its enigmatic nature.
What is Dermatitis Herpetiformis?
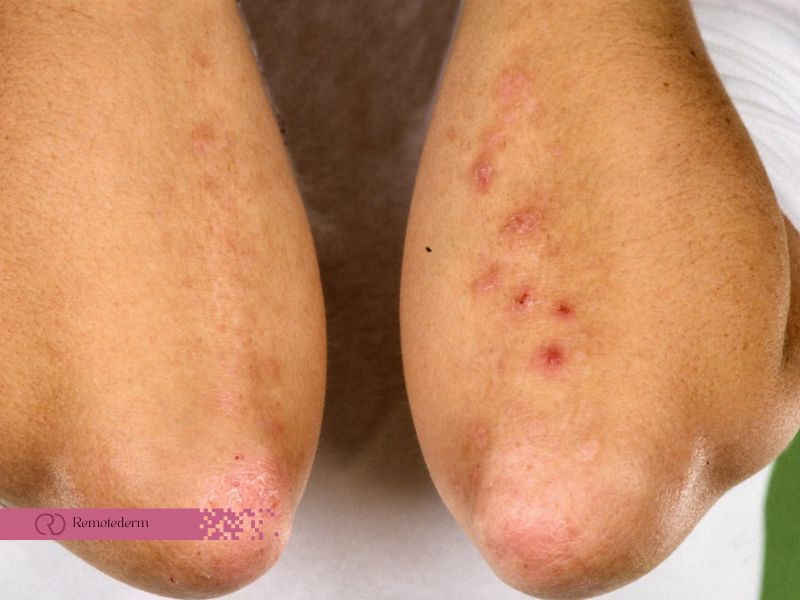
Dermatitis herpetiformis, also known as Duhring’s disease, is a rare, blistering skin condition that manifests as an itchy rash. Despite its name, dermatitis herpetiformis is not related to herpes, but rather it is closely associated with celiac disease, an autoimmune disorder triggered by gluten consumption. The condition is characterized by the presence of small, red bumps and blisters that typically occur symmetrically on the elbows, knees, buttocks, back, and scalp.
Causes and Triggers
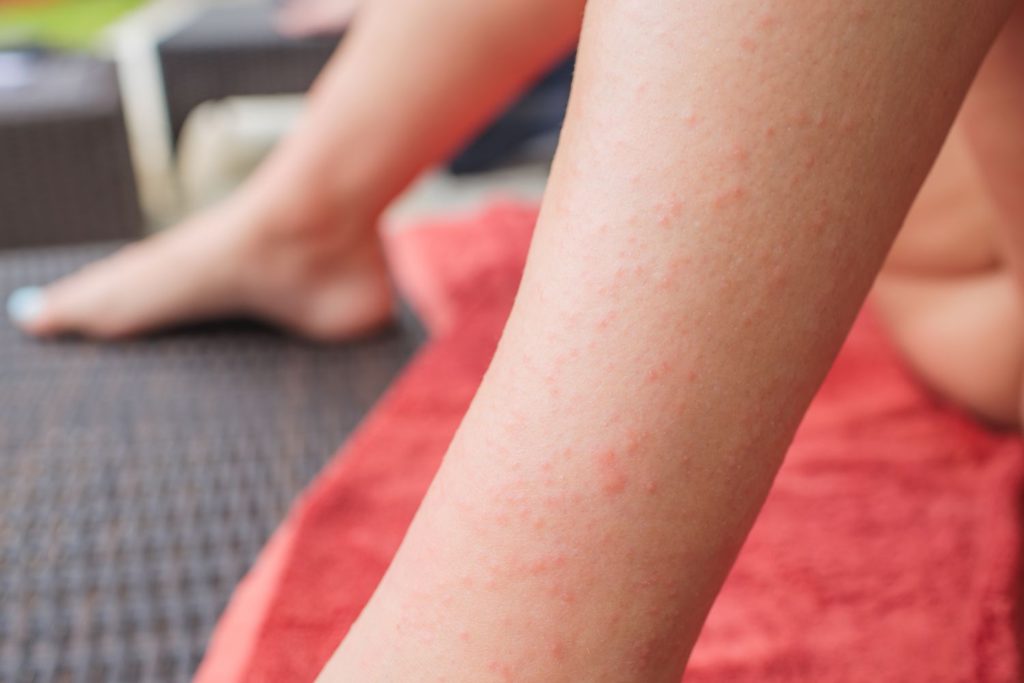
The exact cause of dermatitis herpetiformis remains unknown, but researchers believe it is an immune-mediated response triggered by the ingestion of gluten in genetically predisposed individuals. Gluten, a protein found in wheat, barley, and rye, stimulates an abnormal immune response in people with celiac disease, leading to the deposition of immunoglobulin A (IgA) antibodies in the skin. These antibodies cause inflammation, resulting in the characteristic rash and intense itching.
Symptoms and Diagnosis
The primary symptom of dermatitis herpetiformis is the presence of a persistent, itchy rash characterized by small, fluid-filled blisters and raised red bumps. The rash typically occurs in a symmetrical pattern on the extensor surfaces of the body, such as the elbows, knees, and buttocks. Other common symptoms include a stinging or burning sensation, intense itching, and occasional pain.
To diagnose dermatitis herpetiformis, a dermatologist may perform a skin biopsy, examining a small sample of affected skin under a microscope. The presence of IgA deposits in the skin, along with other characteristic histopathological findings, confirms the diagnosis. Additionally, blood tests may be conducted to detect the presence of specific antibodies associated with celiac disease.
Herpetiformis Dermatitis Treatment Options
The primary treatment for dermatitis herpetiformis involves a strict, lifelong gluten-free diet. By eliminating gluten from their diet, individuals with herpetiformis dermatitis can effectively manage the condition and prevent flare-ups. It is crucial to consult with a registered dietitian or a healthcare professional experienced in celiac disease to ensure a balanced and nutritious gluten-free diet.

In addition to dietary modifications, dermatologists often provide a Dermatitis Herpetiformis prescription to alleviate symptoms and promote healing. The most commonly prescribed medication is dapsone, an oral antibiotic that suppresses the immune response and reduces inflammation. Other medications, such as sulfapyridine, colchicine, and tetracycline, may be prescribed as alternative or adjunct treatments.
Potential Complications
If left untreated or poorly managed, dermatitis herpetiformis can lead to several complications. These may include:
- Intestinal Damage: Dermatitis herpetiformis is closely associated with celiac disease, which can cause significant damage to the small intestine. Over time, this damage may interfere with nutrient absorption and lead to malnutrition.
- Scarring and Hyperpigmentation: Severe or prolonged dermatitis herpetiformis lesions may result in scarring and hyperpigmentation of the affected skin.
- Infections: Continuous scratching of the itchy rash can break the skin barrier, increasing the risk of bacterial infections.
- Psychological Impact: The persistent itchiness and discomfort associated with dermatitis herpetiformis can significantly impact an individual’s quality of life, leading to emotional distress and anxiety.
- Delayed Diagnosis: Due to its rarity and resemblance to other skin conditions, dermatitis herpetiformis is often misdiagnosed or undiagnosed for a considerable period. This delay in diagnosis can prolong the suffering and hinder the initiation of appropriate treatment.
- Nutritional Deficiencies: The strict gluten-free diet required for managing dermatitis herpetiformis may lead to potential nutritional deficiencies, especially if not properly monitored or supplemented.
Please be aware of these potential complications and take the necessary steps to seek timely diagnosis, proper treatment, and ongoing management to minimize their impact and ensure optimal well-being.
Lifestyle Management
Managing dermatitis herpetiformis requires more than just adherence to a gluten-free diet. Consider the following lifestyle management tips to effectively control symptoms and improve overall well-being:
- Education and Support: Educate yourself about celiac disease, dermatitis herpetiformis, and gluten-free living. Seek support from local or online communities to connect with others facing similar challenges.
- Skin Care: Follow a gentle skin care routine to keep the skin clean and moisturized. Avoid harsh soaps, fragrances, and skincare products that may trigger irritation.
- Stress Reduction: Stress can worsen symptoms of dermatitis herpetiformis. Incorporate stress-management techniques such as meditation, yoga, or engaging in hobbies to promote relaxation.
- Clothing and Fabric Choices: Opt for loose-fitting, breathable clothing made from soft, natural fibres like cotton. Avoid synthetic materials that can irritate the skin and exacerbate symptoms. Additionally, be mindful of laundry detergents and fabric softeners, opting for hypoallergenic and fragrance-free options to minimize potential skin reactions.
- Sun Protection: Protect your skin from excessive sun exposure, as it can trigger flare-ups and worsen symptoms. Apply broad-spectrum sunscreen with a high SPF regularly, even on cloudy days. Additionally, seek shade during peak sun hours and wear protective clothing, such as wide-brimmed hats and lightweight long sleeves, to shield your skin from harmful UV rays.
- Regular Follow-ups: Schedule regular follow-up appointments with your dermatologist and healthcare team to monitor your condition, discuss any concerns, and adjust treatment plans if necessary. In addition, consider exploring the convenience and accessibility of Remotederm, an online dermatology consultation service. With Remotederm, you can access professional dermatological advice and guidance from the comfort of your own home, eliminating the need for long waits and in-person visits to dermatologists.

By integrating these lifestyle management tips into your daily routine, you can complement your treatment plan and optimize your skin health while living with dermatitis herpetiformis.
Conclusion
In conclusion, dermatitis herpetiformis is a chronic autoimmune skin condition closely associated with celiac disease. It is essential to understand the causes, symptoms, and available treatment options to effectively manage this condition and improve your quality of life.
By embracing a gluten-free lifestyle and working closely with healthcare professionals, individuals with dermatitis herpetiformis can minimize flare-ups, alleviate symptoms, and prevent potential complications. Adhering to a strict gluten-free diet is crucial, as it plays a fundamental role in managing the condition and promoting overall well-being.
Furthermore, timely diagnosis and proper treatment are essential to prevent long-term damage and mitigate the risk of complications. If you suspect you may have dermatitis herpetiformis, consult with a skin dermatologist experienced in autoimmune skin conditions.
FAQs
- Is dermatitis herpetiformis contagious?
No, dermatitis herpetiformis is not contagious. It is an autoimmune skin condition and cannot be transmitted from person to person.
- Can dermatitis herpetiformis spread to other parts of the body?
While dermatitis herpetiformis can occur in different areas of the body, it does not spread from one person to another.
- How is dermatitis herpetiformis diagnosed?
Dermatitis herpetiformis is typically diagnosed through a skin biopsy and blood tests to detect specific antibodies associated with celiac disease.
- Can dermatitis herpetiformis be treated with medication alone?
Medication, such as dapsone, is often prescribed to manage symptoms, but a lifelong gluten-free diet is also necessary for effective treatment.
- Is dermatitis herpetiformis curable?
While there is no cure for dermatitis herpetiformis, it can be effectively managed through a gluten-free diet and appropriate treatment.