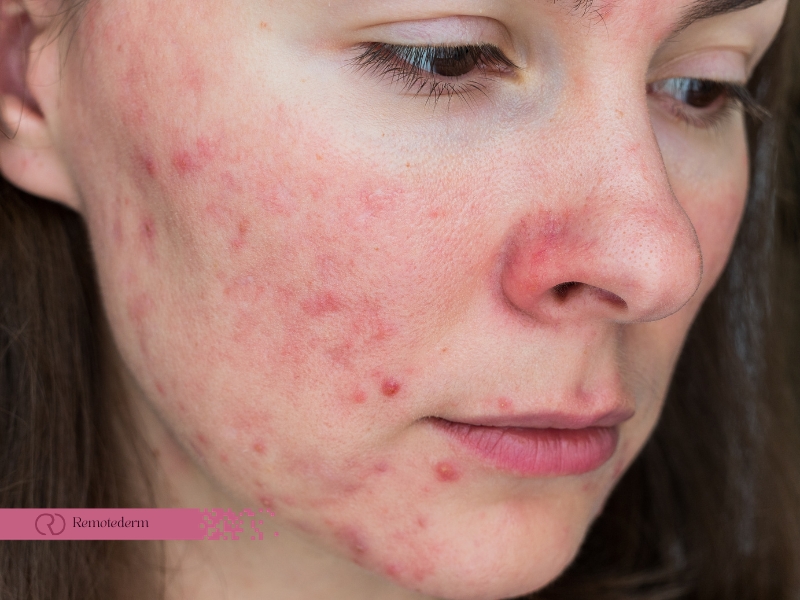
Papulopustular rosacea is a common and distressing skin condition that affects millions of individuals worldwide. It is a subtype of rosacea, a chronic dermatological disorder characterized by redness, inflammation, and visible blood vessels primarily on the central face. In this comprehensive guide, we will delve deep into the complexities of papulopustular rosacea, exploring its causes, triggers, symptoms, available treatment options, and the benefits of consulting an online dermatologist.
Understanding Papulopustular Rosacea
Papulopustular rosacea is a subtype of rosacea, and similar to rosacea, the exact cause of it is unknown. However, it is believed to be caused by a combination of genetic, environmental, and immunological factors. Rosacea is more common in people with fair skin, but it can affect people of all skin types and ethnic backgrounds.
Symptoms of Papulopustular Rosacea
Papulopustular rosacea is characterized by the following symptoms:
- Redness (Erythema): Persistent facial redness, medically termed erythema, is one of the most distinctive and pervasive symptoms of papulopustular rosacea. This redness usually affects the central face, encompassing the cheeks, nose, and forehead. It can lead to discomfort and self-consciousness.
- Papules: The appearance of small, raised, red bumps known as papules is a common symptom. These papules can be sensitive, itchy, or tender to the touch, contributing to an uneven and irritated complexion.
- Pustules: Pustules are small, pus-filled bumps that resemble acne pimples. They may become more conspicuous during rosacea flare-ups, adding to the overall discomfort and cosmetic concerns.
- Flushing: Intermittent episodes of facial flushing can cause the skin to turn red and feel warm. Flushing is often triggered by various stimuli, such as spicy foods, alcohol, or emotional stress.
- Telangiectasia: Visible blood vessels, known as telangiectasia, can appear on the facial skin, further intensifying the overall redness. These blood vessels can be prominent and distressing for many individuals.
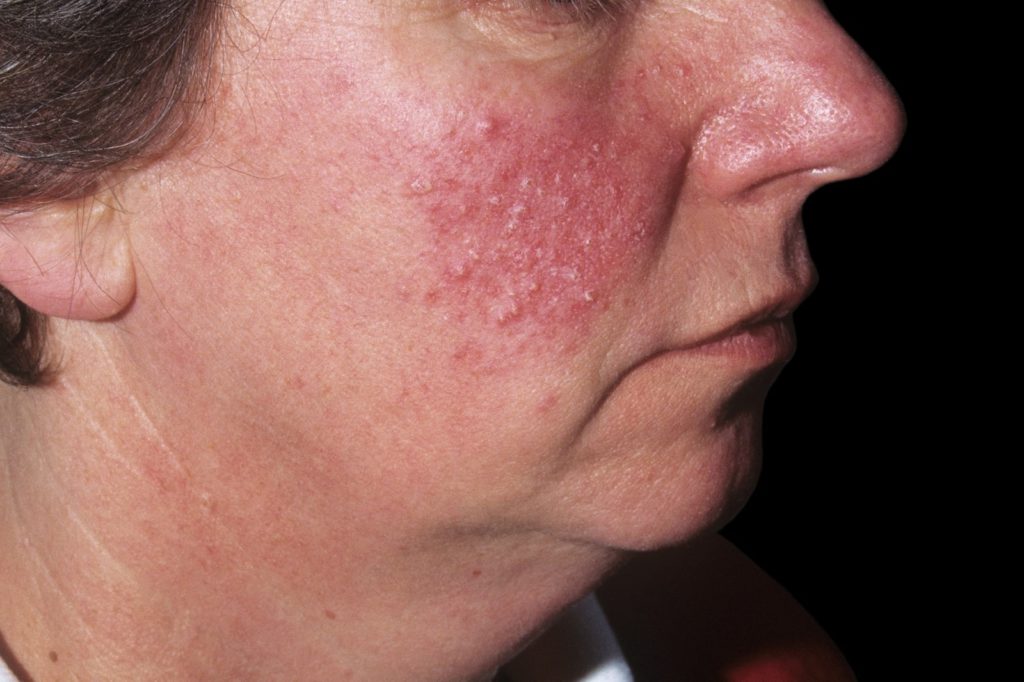
Papulopustular Rosacea Triggers
Identifying and avoiding triggers plays a pivotal role in the comprehensive management of papulopustular rosacea. While these triggers can vary from person to person, understanding the common culprits that exacerbate rosacea symptoms is essential. Let’s explore these triggers in greater detail:
- Sun Exposure: Exposure to ultraviolet (UV) rays is a well-known and prevalent exacerbating factor for rosacea symptoms. The sun’s rays can intensify redness and inflammation. To shield the skin from UV damage, it’s imperative to practice proper sun protection. This involves using sunscreen with a high Sun Protection Factor (SPF) and wearing protective clothing, including wide-brimmed hats and sunglasses.
- Extreme Temperatures: The weather can be a formidable foe for those with rosacea. Both extreme cold and hot weather conditions can provoke flare-ups. Cold weather can cause skin to become dry and irritated, while excessive heat can lead to flushing and increased redness. To mitigate these effects, dressing appropriately for the weather and using humidifiers or fans to maintain a comfortable indoor environment can be beneficial.
- Spicy Foods: Spicy foods, hot beverages, and alcohol consumption are well-documented as common culprits in causing flushing and exacerbating rosacea symptoms. Capsaicin, the compound responsible for the heat in chili peppers, is a known trigger. Reducing or avoiding these triggers in your diet can significantly improve the condition and provide relief.
- Certain Skincare Products: Harsh skincare products can be a double-edged sword for those with papulopustular rosacea. Products that contain alcohol, fragrances, or other irritating ingredients can exacerbate skin sensitivity and worsen rosacea symptoms. Opting for gentle, fragrance-free skincare products that focus on soothing and hydrating the skin can help minimize irritation and improve overall skin health.
- Stress: Emotional stress, a common companion in our fast-paced lives, can be a major factor in triggering rosacea flare-ups. The mind-skin connection is well-established, and stress can lead to the release of certain neurotransmitters and hormones that dilate blood vessels and intensify redness. Stress management is a crucial part of rosacea care. Techniques such as yoga, meditation, deep breathing exercises, and mindfulness can help reduce stress-related triggers and enhance overall well-being.
- Medications: While medications can be necessary for various medical conditions, it’s important to be aware that some medications, particularly topical steroids, can exacerbate rosacea symptoms. If you suspect that your medication may be contributing to your symptoms, it is essential to consult a dermatologist or healthcare provider. They can work with you to find alternative treatment options that do not worsen your rosacea.
Treatment Options for Papulopustular Rosacea
While there is no cure for papulopustular rosacea, numerous treatment options are available to manage its symptoms effectively:
- Topical Medications: Topical creams or gels containing active ingredients like metronidazole, azelaic acid, or ivermectin can help reduce redness, papules, and pustules when applied once or twice a day.
- Oral Antibiotics: For more severe cases, oral antibiotics such as doxycycline, tetracycline, or minocycline may be prescribed to reduce inflammation and control the condition.
- Laser Therapy: Laser and light-based treatments can target visible blood vessels (telangiectasia) and reduce redness. Multiple sessions may be required for optimal results.
- Topical Calcineurin Inhibitors: Topical medications like tacrolimus and pimecrolimus, which are immunosuppressive agents, can help control inflammation and redness.
- Skincare Routine: A gentle skincare routine that avoids harsh ingredients can help minimize irritation and flare-ups. Using a mild cleanser, moisturizer, and sunscreen daily is crucial.

- Lifestyle Adjustments: Making lifestyle changes, such as avoiding triggers and managing stress effectively, are essential for long-term rosacea management.
Consulting an Online Dermatologist for Rosacea
If you’re struggling to manage your papulopustular rosacea, consulting with a rosacea online dermatologist can be a convenient and effective way to receive personalized guidance and treatment recommendations. Online dermatologists can assess your condition, recommend suitable treatments, and provide ongoing support and monitoring, all from the comfort of your home.
Final Thoughts
Papulopustular rosacea, a subtype of rosacea, can be challenging. It’s characterized by symptoms like redness, papules, pustules, flushing, and visible blood vessels. While its precise cause is unclear, it’s likely influenced by genetics, environment, and immune responses.
Managing papulopustular rosacea involves understanding triggers like sun exposure, extreme temperatures, spicy foods, harsh skincare products, stress, and some medications. By avoiding these triggers and adopting a gentle skincare routine, individuals can reduce flare-ups.
Topical medications, oral antibiotics, laser therapy, topical calcineurin inhibitors, and lifestyle changes are among the treatment options. A convenient option is to consult an online dermatologist for personalized advice.
In conclusion, papulopustular rosacea can be managed with the right knowledge and approach. By controlling triggers, adopting appropriate treatments, and making lifestyle adjustments, individuals can transform redness into radiance with the support of healthcare professionals and resources.
FAQs
- Are oral antibiotics effective for papulopustular rosacea?
Yes, oral antibiotics such as doxycycline or minocycline are often prescribed to reduce inflammation.
- Can people with papulopustular rosacea use makeup?
Yes, gentle, non-comedogenic makeup can be used to conceal redness and imperfections.
- Is papulopustular rosacea more common in men or women?
It’s more common in women, but men can also be affected.
- Can papulopustular rosacea affect the eyes?
Yes, ocular rosacea can occur in conjunction with skin symptoms and affect the eyes.