Many people struggle with hair loss and scalp discomfort, often unaware of the underlying cause – Lichen Planopilaris (LPP). We’ll delve into the complex world of Lichen Planopilaris, a chronic inflammatory condition that can affect anyone, unravelling its symptoms, causes, and the most recent treatment options available. Understanding LPP is the first step toward unlocking the secret to healthier, happier hair, whether you’re looking for answers for yourself or someone you care about. So, let’s go on this adventure together and find the solutions that can transform your hair and your confidence.
Understanding Lichen Planopilaris
Lichen Planopilaris (LPP) is a chronic inflammatory condition that affects the hair follicles, leading to hair loss and scalp discomfort. This relatively rare disorder falls under the broader category of scarring alopecia, where hair follicles are progressively destroyed, replaced by scar tissue, and consequently unable to regrow hair. Understanding Lichen Planopilaris is essential for both patients and healthcare professionals to facilitate early diagnosis and appropriate management.
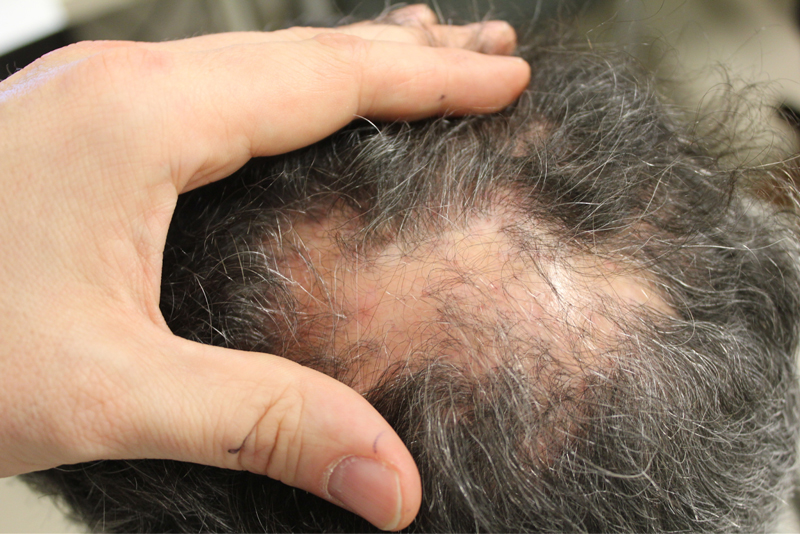
Lichen Planopilaris Symptoms
Lichen Planopilaris (LPP) manifests through various symptoms, often affecting the scalp, and occasionally other areas of the body. Common symptoms of lichen planopilaris scalp include:
- Hair Loss: One of the primary indications of LPP is progressive hair loss, which may start as a small, isolated patch and gradually spread across the scalp.
- Itchy or Burning Scalp: Many individuals with LPP experience itching or a burning sensation on the affected scalp, which can be quite uncomfortable.
- Red or Inflamed Bumps: LPP often presents as small, reddish or purplish bumps on the scalp, resembling pimples or pustules.
- Scaling or Flaking: The affected scalp may develop scales or flakes, similar to dandruff, which can sometimes be mistaken for other scalp conditions.
- Scarring: Over time, LPP can lead to scarring of the scalp, resulting in permanent hair loss and a smooth, shiny appearance in affected areas.
- Tenderness: Some individuals may notice tenderness or pain in the affected scalp regions.
If you have these symptoms, you should see a dermatologist right away because early diagnosis and treatment can help manage LPP and minimize hair loss and scarring.
Causes of Lichen Planopilaris
The exact causes of Lichen Planopilaris (LPP) remain unclear, but it is believed to be a complex interplay of genetic, autoimmune, and environmental factors. Several potential causes and contributing factors have been identified, including:
- Autoimmune Response: LPP is thought to involve an autoimmune response, where the body’s immune system mistakenly targets and attacks hair follicles, leading to inflammation and damage.
- Genetic Predisposition: Genetics may play a role, as LPP tends to run in families, suggesting a genetic susceptibility to the condition.
- Environmental Triggers: Certain environmental factors may trigger or exacerbate LPP in susceptible individuals. These factors can include stress, infections, medications, and even physical trauma to the scalp.
- Inflammatory Pathways: Aberrant inflammatory pathways within the scalp may contribute to the development and progression of LPP.
- Hormonal Changes: In some cases, hormonal changes, such as those experienced during menopause, may influence the onset or severity of LPP.
- Other Medical Conditions: LPP has been associated with other autoimmune conditions, such as lupus or lichen planus in other parts of the body, suggesting a potential connection between these conditions.
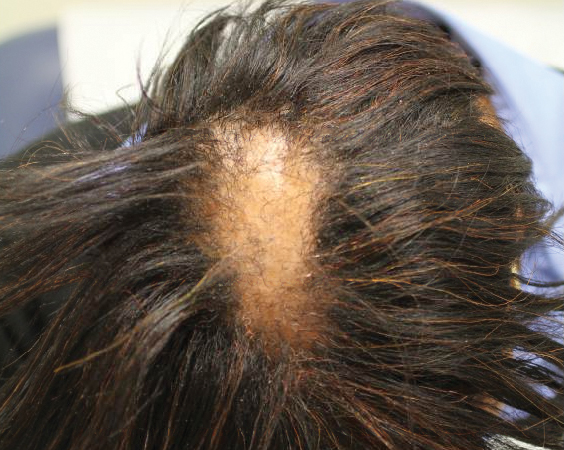
While these factors may contribute to the development of Lichen Planopilaris, further research is needed to fully understand the precise mechanisms behind this condition. Identifying the causes is crucial for developing more effective treatments and prevention strategies.
Diagnosis of Lichen Planopilaris
Diagnosing LPP often requires a biopsy to examine scalp tissue under a microscope, as it can mimic other hair loss conditions. Early detection is crucial, as prompt intervention can help slow or halt the progression of the disease. Treatment options for LPP may include topical or oral corticosteroids, immunosuppressants, or anti-inflammatory medications. Hair restoration techniques like hair transplantation may be considered once the inflammation is under control.
Living with Lichen Planopilaris can be emotionally challenging due to its impact on appearance and self-esteem. Support groups and counselling can provide valuable emotional support and coping strategies for individuals affected by this condition.
Can Lichen Planopilaris Be Cured?
The million-dollar question for anyone dealing with lichen planopilaris is whether there’s a cure. Unfortunately, lichen planopilaris is a chronic condition, and there is no known cure at present. This, however, does not mean that all hope is lost. Various treatments can help manage the symptoms and potentially slow down hair loss.
Treatment Options for Lichen Planopilaris
Treatment options for Lichen Planopilaris (LPP) aim to alleviate symptoms, manage inflammation, and slow down the progression of the disease. Depending on the severity of the condition and individual response, various treatment approaches can be considered:
- Corticosteroids: These can be administered topically (creams or ointments) or orally (pills). Corticosteroids are potent anti-inflammatory medications that help reduce redness, itching, and inflammation in the affected areas of the scalp. They may also suppress the overactive immune response responsible for LPP. However, long-term use of oral corticosteroids should be carefully monitored due to potential side effects.
- Topical Calcineurin Inhibitors: When corticosteroids are ineffective or not well-tolerated, topical calcineurin inhibitors like tacrolimus or pimecrolimus may be prescribed. These medications also help reduce inflammation and can be particularly useful for sensitive areas like the face or neck.
- Oral Retinoids: In some cases, oral retinoids, such as isotretinoin, may be recommended to manage LPP. These drugs modulate the immune response and control inflammation, potentially slowing hair loss progression.
- Laser Therapy (LLLT): Low-level laser therapy has emerged as a promising treatment option for LPP. LLLT devices emit low-level laser light that stimulates hair follicles and promotes hair regrowth. While its efficacy may vary among individuals, some patients have experienced positive results.
- Immunosuppressants: In severe or rapidly progressing cases of LPP, immunosuppressant medications like methotrexate or cyclosporine may be considered. These drugs work to suppress the immune system’s activity, preventing further damage to hair follicles.
It’s crucial to consult a dermatologist or healthcare professional for a personalized treatment plan tailored to the individual’s specific LPP symptoms and needs. Treatment outcomes can vary, and periodic monitoring is essential to assess progress and adjust therapies as necessary.
Seeking Help from a Hair Loss Dermatologist in Canada
Dealing with lichen planopilaris can be challenging, but you don’t have to face it alone. In Canada, there are experienced dermatologists who specialize in treating hair loss conditions. Here are some steps to help you find the right hair loss dermatologist Canada:
- Research: Start by researching dermatologists in your area who specialize in hair loss conditions. Look for reviews, recommendations, and qualifications.
- Consultation: Schedule a consultation with a dermatologist who has experience in treating lichen planopilaris.
- Ask Questions: Don’t hesitate to ask questions about the dermatologist’s experience, success rates with lichen planopilaris patients, and any concerns you may have.
- Treatment Plan: Work with your dermatologist to create a treatment plan that is unique to your condition and needs. Make sure to closely follow their recommendations.

Can You Dye Your Hair If You Have Lichen Planopilaris?
Dyeing your hair can be a concern if you have lichen planopilaris, as the chemicals in hair dye can potentially worsen the condition or cause skin reactions. Consider the following key points:
- Patch Test: Before dyeing your hair, perform a patch test to check for any adverse reactions. Apply a small amount of the dye to a discreet area of your skin, wait for the recommended time, and assess for redness, itching, or irritation.
- Consult Your Dermatologist: It’s advisable to consult your dermatologist before using hair dye. They can provide personalized guidance based on your specific condition and recommend hair dye products that are less likely to trigger adverse reactions.
- Choose Gentle Formulas: Opt for hair dye products that are free from harsh chemicals and ammonia. Semi-permanent or vegetable-based dyes may be gentler on the scalp.
- Monitor Your Scalp: After dyeing your hair, keep a close eye on your scalp for any signs of irritation or worsening of lichen planopilaris symptoms. If you notice any issues, discontinue use immediately and seek medical advice.
Final Thoughts
Living with lichen planopilaris can be challenging, but with the right information and guidance, you can effectively manage the condition and maintain healthy hair. While there may not be a cure for lichen planopilaris, various treatment options and precautions can help you minimize its impact on your scalp and overall well-being.
Remember, it’s essential to consult with a dermatologist who specializes in hair loss conditions to receive personalized care and support. By taking proactive steps and staying informed, you can unlock the secret to healthy hair even in the face of lichen planopilaris.
FAQs
- Can LPP affect other parts of the body besides the scalp?
LPP can occasionally affect other areas of the body but primarily manifests on the scalp.
- Is it safe to use topical corticosteroids for LPP long-term?
Long-term use should be monitored due to potential side effects, and it’s essential to follow your dermatologist’s guidance.
- Are there alternative therapies for Lichen Planopilaris?
Some individuals have found relief through low-level laser therapy (LLLT) and may consider hair transplantation once inflammation is under control.
- Does LPP run in families?
Yes, genetics may play a role, as LPP tends to have a familial component, suggesting a genetic predisposition.
