Eczema vs psoriasis: what’s the difference? Skin conditions can be frustrating and uncomfortable, but they are also incredibly common. Eczema and psoriasis are two chronic skin conditions that affect millions of people worldwide. While these conditions may share some similarities, such as causing red, scaly patches of skin and intense itching, there are also some key differences between the two. In this article, we will explore the similarities and differences between eczema and psoriasis, including their causes, symptoms, and treatments. We will also provide some helpful tips for managing these conditions and provide photos to aid in diagnosis. If you or a loved one is living with eczema or psoriasis, read on to learn more.
What is Eczema?
Atopic dermatitis, or eczema, is a chronic skin condition that results in red, itchy, and inflamed skin. Although it can affect anyone, children are the most frequently affected. Eczema is linked to allergies and asthma and frequently runs in families.
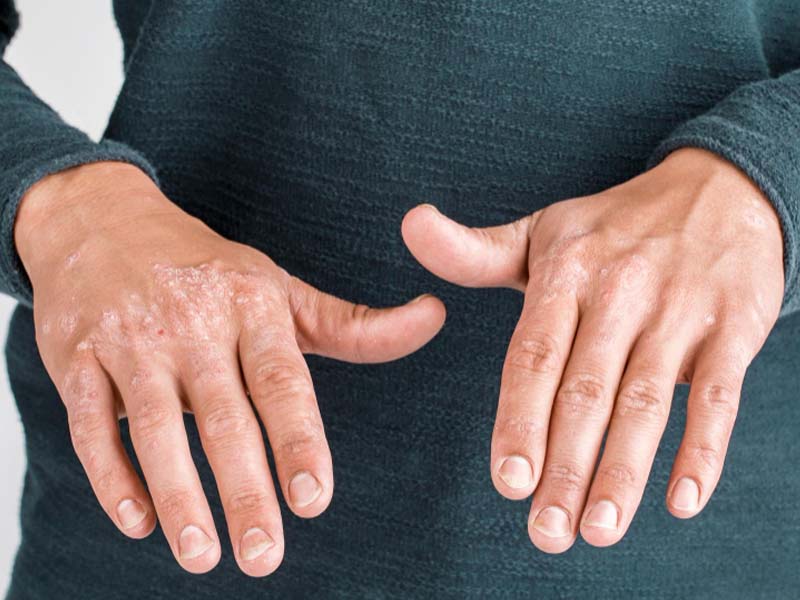
Symptoms of eczema include dry, scaly patches of skin, intense itching, redness, and inflammation. The affected areas may also become thickened or develop blisters that ooze and crust over. Eczema can appear on any part of the body, but it most commonly affects the hands, face, neck, and legs.
Causes of Eczema
The exact cause of eczema is still unknown, but research suggests that it is a combination of genetic and environmental factors that contribute to the development of the condition. Here are some of the factors that are believed to trigger or worsen eczema:
- Genetic factors: Eczema tends to run in families, and people with a family history of eczema, asthma, or hay fever are more likely to develop the condition.
- Environmental factors: Exposure to certain environmental factors can trigger eczema or worsen existing symptoms. These factors include:
- Allergens: Common allergens that can trigger eczema include foods, pollen, dust mites, and pet dander.
- Irritants: Chemicals, soaps, detergents, and other irritants can cause eczema to flare up.
- Climate: Extreme temperatures, low humidity, and dry or cold weather can dry out the skin and trigger eczema.
- Stress: Emotional stress and anxiety can trigger eczema or make existing symptoms worse by affecting the immune system and skin barrier function.
Identifying and avoiding triggers is an important part of managing eczema, as it can help reduce the frequency and severity of flare-ups. In addition to avoiding triggers, using gentle skin care products, moisturizing regularly, and following a healthy lifestyle can also help manage symptoms.
If you or someone you know is struggling with eczema, click on the link to learn more about the causes, symptoms, and treatment options available. Don’t suffer in silence – there are ways to manage eczema and get relief from the symptoms.
What is Psoriasis?
Psoriasis is a chronic autoimmune disease that causes the skin cells to multiply faster than normal, resulting in the buildup of thick, scaly patches of skin. It can affect people of all ages, but adults are the most commonly affected. Psoriasis is not contagious and cannot be transmitted from one person to another.
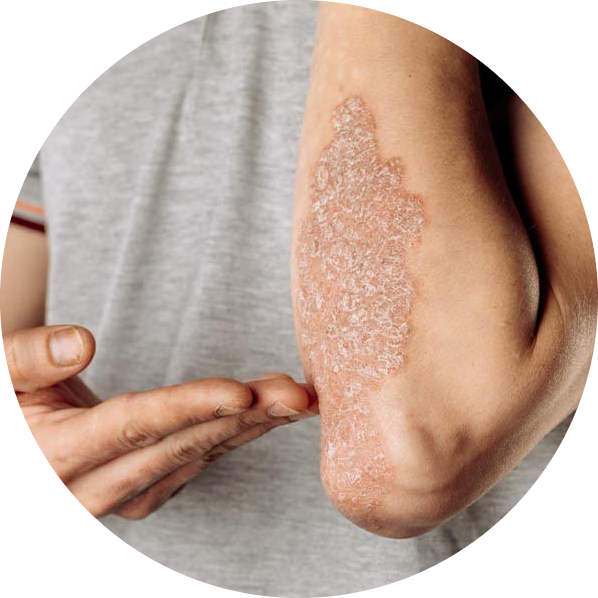
Symptoms of psoriasis include red, raised patches of skin with silvery scales, itching and burning, and sometimes even pain. Psoriasis can appear on any part of the body, but it is most commonly found on the scalp, elbows, knees, and lower back.
Causes of Psoriasis
Psoriasis is a chronic autoimmune condition that affects the skin and joints. The exact cause of psoriasis is unknown, but it is believed to be a combination of genetic and environmental factors. People with psoriasis have an overactive immune system that mistakenly attacks healthy skin cells, leading to inflammation and the rapid growth of skin cells. Some of the factors that can trigger or worsen psoriasis include:
- Infections such as strep throat or skin infections: These can cause psoriasis to flare up or worsen.
- Stress and emotional upheaval: Stress can trigger psoriasis flare-ups or make existing symptoms worse.
- Certain medications such as beta-blockers and lithium: These medications can cause psoriasis or worsen existing symptoms.
- Injury to the skin, such as cuts or burns: Injured skin can trigger psoriasis symptoms in the affected area.
To help manage symptoms of psoriasis, it’s crucial to identify and avoid triggers that can worsen the condition. Along with that, proper treatment can significantly reduce inflammation, itching, and discomfort associated with psoriasis. We’ve put together a comprehensive guide to help you better understand psoriasis and what you can do to manage it.
Eczema vs Psoriasis: What’s the Difference?
Eczema and psoriasis are common skin conditions that can significantly impact an individual’s daily life. Both are chronic conditions that cause discomfort and can negatively affect one’s quality of life. While eczema and psoriasis share some similarities, including the fact that they both involve inflammation of the skin, there are also some distinct differences between the two conditions. Understanding these differences can help individuals better manage their symptoms and seek appropriate treatment.
- One of the most noticeable differences between eczema and psoriasis is their appearance. Eczema typically appears as red, scaly patches of skin, while psoriasis appears as thick, raised, silver or white patches of skin.
- Additionally, the location of the patches can differ between the two conditions. Psoriasis is commonly found on the scalp, elbows, knees, and lower back, while eczema is commonly found on the hands, neck, and legs.
- Another difference is the level of itching or pain associated with the conditions. Eczema is often itchy, while psoriasis can be painful and burning.
- The age of onset also differs between the two conditions, with eczema often appearing in childhood and psoriasis being more common in adults.

Diagnosing Eczema vs Psoriasis
Diagnosing eczema and psoriasis typically involves a physical examination of the skin and a review of the patient’s medical history.
After the initial physical examination and review of medical history, there are additional diagnostic tests that can help distinguish between eczema and psoriasis. One such test is a patch test, which involves applying small patches of different substances to the skin to identify possible triggers of eczema. Blood tests may also be conducted to rule out other conditions that could be causing similar symptoms.

In some cases, a dermatologist may use a tool called a dermoscope to examine the skin more closely. This non-invasive procedure allows the dermatologist to magnify the affected area and observe the skin’s structure and patterns, aiding in the diagnosis.
Overall, accurate diagnosis of eczema and psoriasis is essential for effective treatment. If you suspect you have either condition, it is important to seek medical attention from a dermatologist who can properly diagnose the condition and provide appropriate treatment.
Eczema and Psoriasis Treatment
Eczema and psoriasis are chronic conditions that cannot be cured, but proper treatment can help manage symptoms and improve quality of life. The treatment for eczema and psoriasis often involves a combination of lifestyle changes, medications, and topical treatments.
- Lifestyle changes such as avoiding triggers like irritants, allergens, and stress can help reduce flare-ups of eczema and psoriasis. Patients should also moisturize regularly and avoid hot showers, as they can dry out the skin and exacerbate symptoms. It is important for patients to identify their triggers and take steps to avoid them.
- Medications may be prescribed to help manage symptoms of eczema and psoriasis. Antihistamines and corticosteroids can help reduce inflammation and itching in patients with eczema and psoriasis. Immunosuppressants may also be prescribed in some cases to help control symptoms. In severe cases, biologic drugs that target specific parts of the immune system may also be prescribed.
- Topical treatments such as moisturizers, creams, and ointments can help soothe and hydrate the skin. They are often used as a first line of treatment for mild to moderate cases of eczema and psoriasis. Other topical treatments, such as salicylic acid, coal tar, and vitamin D analogues, may also be used to help reduce inflammation and itching. These treatments work by slowing down the growth of skin cells and reducing inflammation.

Psoriasis vs Eczema Photos
Pictures can be helpful in distinguishing between eczema and psoriasis. Eczema photos typically show red, scaly patches of skin, while psoriasis photos show thick, raised, silver or white patches of skin.

Final Thoughts
Understanding the differences between eczema and psoriasis is essential if you or a loved one suffer from either of these conditions. You should also seek the right medical care. While both conditions have the potential to be uncomfortable and have a negative impact on a person’s quality of life, they vary noticeably in terms of how they look, where they are, and how itchy or painful they are.

It is recommended that you consult a dermatologist for a proper diagnosis and treatment plan if you are exhibiting symptoms of eczema or psoriasis. Remotederm, a service that offers online dermatology consultation and accessible, reasonably priced care from the comfort of your home, is one practical choice. Without leaving their home, patients can use Remotederm to get a diagnosis, a treatment plan, and a prescription.
Identifying and avoiding triggers, using gentle skin care products, moisturizing frequently, maintaining a healthy lifestyle, and receiving the appropriate medical care are all necessary for managing the symptoms of eczema or psoriasis. Eczema and psoriasis sufferers can lead comfortable, healthy lives with the right care.
FAQs
1. Are Eczema and Psoriasis similar?
No, while both conditions can cause skin discomfort, they are different in terms of appearance, location on the body, and the level of itching or pain they cause. Eczema is usually found in areas where the skin creases, while psoriasis is commonly found on the scalp, knees, and elbows.
2. Are eczema and psoriasis contagious?
No, neither eczema nor psoriasis is contagious. They are both chronic skin conditions that are not caused by a virus or bacteria.
3. Can eczema turn into psoriasis?
No, eczema and psoriasis are two distinct skin conditions that do not turn into each other. However, they may both occur in the same individual.
4. Can stress cause eczema or psoriasis?
Yes, stress is a common trigger for both eczema and psoriasis. Managing stress through relaxation techniques and other methods may help reduce flare-ups.
5. How do I know if I have eczema or psoriasis?
If you’re experiencing symptoms such as redness, itching, scaling, or flaking skin, it’s recommended to consult a dermatologist for a proper diagnosis.
6. Is it possible to prevent eczema or psoriasis?
There is no guaranteed way to prevent eczema or psoriasis, but avoiding triggers and following a healthy lifestyle can help reduce the likelihood of developing these conditions or experiencing flare-ups.
